 Your new post is loading...
 Your new post is loading...
For individuals experiencing lower back pain can understanding the anatomy and function of the multifidus muscle help in injury prevention and in the development of a highly effective treatment plan? Multifidus Muscle The multifidus muscles are long and narrow on either side of the spinal column, which helps stabilize the lower region of the spine or lumbar spine. (Maryse Fortin, Luciana Gazzi Macedo 2013) Sitting too much, practicing unhealthy postures, and lack of movement can progress to the multifidus muscle weakening or atrophy, which can lead to spinal instability, vertebral compression, and back pain. (Paul W. Hodges, Lieven Danneels 2019) Anatomy Known as the deep layer, it is the innermost layer of the three muscle layers of the back and controls the movement of the spine. The other two layers, known as the intrinsic and superficial, are responsible for the thoracic cage/rib cage and shoulder movement. (Anouk Agten et al., 2020) The multifidus has attachment points at: - The thoracic spine of the middle back.
- The lumbar spine of the lower back.
- The iliac spine - the base of the wing-shaped iliac bone of the pelvis.
- Sacrum - series of bones at the base of the spine connected to the tailbone.
- When standing or moving, the multifidus muscle works with the transversus abdominus and pelvic floor muscles to stabilize the lumbar spine. (Christine Lynders 2019)
Muscle Function The main function is to stabilize the lower back, but it also helps extend the lower spine whenever reaching or stretching. (Jennifer Padwal et al., 2020) Because the muscle has numerous attachment points and is serviced by a specific branch of nerves known as the posterior rami, it allows each vertebra to work individually and more efficiently. - This protects against spinal deterioration and the development of arthritis. (Jeffrey J Hebert et al., 2015)
- The multifidus muscle works with two other deep muscle groups to stabilize and move the spine. (Jeffrey J Hebert et al., 2015)
- The rotatores muscle enables unilateral rotation, turning from side to side, and bilateral extension or bending backward and forward.
- The semispinalis muscle above the multifidus allows extension and rotation of the head, neck, and upper back.
- The multifidus muscle ensures spinal strength because it has more attachment points to the spine than the other layers, which reduces spinal flexibility and rotation but increases strength and stability. (Anouk Agten et al., 2020)
Lower Back Pain A weak multifidus muscle destabilizes the spine and provides less support to the vertebra. This adds pressure on muscles and connective tissues between and adjacent to the spinal column, increasing the risk of lower back pain symptoms. (Paul W. Hodges, Lieven Danneels 2019) The loss of muscle strength and stability can cause atrophy or wasting away. This can cause compression and other back problems. (Paul W. Hodges et al., 2015) Back problems associated with multifidus muscle deterioration include (Paul W. Hodges, Lieven Danneels 2019) - Herniated discs - also bulging or slipped discs.
- Nerve entrapment or compression pinched nerve.
- Sciatica
- Referred pain - nerve pain originating from the spine felt in other areas.
- Osteoarthritis - wear-and-tear arthritis
- Spinal osteophytes - bone spurs
- Weak abdominal or pelvic floor muscles can compromise the core, increasing the risk of chronic lower back pain and injury.
Individuals are recommended to consult a physical therapist and chiropractor who can help develop the appropriate treatment, rehabilitation, and strengthening plan based on age, injury, underlying conditions, and physical abilities. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research studies or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please contact Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Fortin, M., & Macedo, L. G. (2013). Multifidus and paraspinal muscle group cross-sectional areas of patients with low back pain and control patients: a systematic review with a focus on blinding. Physical therapy, 93(7), 873–888. https://doi.org/10.2522/ptj.20120457 Hodges, P. W., & Danneels, L. (2019). Changes in Structure and Function of the Back Muscles in Low Back Pain: Different Time Points, Observations, and Mechanisms. The Journal of orthopedic and sports physical therapy, 49(6), 464–476. https://doi.org/10.2519/jospt.2019.8827 Agten, A., Stevens, S., Verbrugghe, J., Eijnde, B. O., Timmermans, A., & Vandenabeele, F. (2020). The lumbar multifidus is characterized by larger type I muscle fibers compared to the erector spinae. Anatomy & cell biology, 53(2), 143–150. https://doi.org/10.5115/acb.20.009 Lynders C. (2019). The Critical Role of Development of the Transversus Abdominis in Preventing and Treatment Low Back Pain. HSS journal: The Musculoskeletal Journal of Hospital for Special Surgery, 15(3), 214–220. https://doi.org/10.1007/s11420-019-09717-8 Padwal, J., Berry, D. B., Hubbard, J. C., Zlomislic, V., Allen, R. T., Garfin, S. R., Ward, S. R., & Shahidi, B. (2020). Regional differences between superficial and deep lumbar multifidus in patients with chronic lumbar spine pathology. BMC musculoskeletal disorders, 21(1), 764. https://doi.org/10.1186/s12891-020-03791-4 Hebert, J. J., Koppenhaver, S. L., Teyhen, D. S., Walker, B. F., & Fritz, J. M. (2015). The evaluation of lumbar multifidus muscle function via palpation: reliability and validity of a new clinical test. The Spine Journal: official North American Spine Society journal, 15(6), 1196–1202. https://doi.org/10.1016/j.spinee.2013.08.05 Hodges, P. W., James, G., Blomster, L., Hall, L., Schmid, A., Shu, C., Little, C., & Melrose, J. (2015). Multifidus Muscle Changes After Back Injury Are Characterized by Structural Remodeling of Muscle, Adipose and Connective Tissue, but Not Muscle Atrophy: Molecular and Morphological Evidence. Spine, 40(14), 1057–1071. https://doi.org/10.1097/BRS.0000000000000972
The NHTSA records show that rear-end collisions are the most common and make up 30% of all traffic accidents, crashes, and collisions. Rear-end collisions can come out of nowhere. One moment a driver is waiting at a stop or light, and suddenly they are catapulted forward by the intense force of another vehicle/s resulting in serious and sustaining injuries that can impact an individual's physical capabilities. Rear-end collision injuries most commonly affect the neck and back. This is because of the excessive force and intense shifting and whipping the body goes through. Chiropractic care, massage, and decompression therapy can realign the body, relax the muscles, release compressed nerves, expedite recovery, and restore mobility and function. Rear-End Collision Injuries Rear-end collision injuries can range from mild to serious, and what seems like a minor pull can result in a severe injury. The most common injuries include: - Contusions
- Neck and spinal injuries
- Whiplash
- Concussion
- Traumatic brain and other head injuries.
- Facial injuries
- Dental injuries
- Lacerations
- Broken bones
- Crushed or fractured ribs
- Punctured lungs
- Internal bleeding
- Paralysis
- Pre-existing conditions such as degenerative disc disease can worsen.
Collision Types A rear-end collision can occur in several ways. The most common types include: Tailgating - When drivers in the rear follow another motorist too closely, and the lead motorist slows down or has to stop quickly, the rear driver hits the vehicle because there was not enough adequate time and distance to stop.
Slow Speed Collisions - Slow-speed/low-impact collisions or fender benders can result in spinal injuries and concussions.
- They can also lead to facial and head injuries from sudden airbag deployment.
Vehicle Pile-Ups - A single rear-end collision on a busy street or interstate highway can cause a chain reaction of multiple-vehicle collisions.
- These accidents can cause devastating injuries.
Causes Causes that can take attention away from the road include: - Speeding
- Distracted driving - Talking or texting.
- Tailgating
- Looking at something like an accident while driving by.
- Unsafe lane changes
- Drowsy or fatigued driving
- Construction site hazards
- Poor weather conditions
- Parking lot accidents
Chiropractic Care Symptoms of rear-end collision injuries may not immediately present following an accident. It can take 24 to 48 hours for discomfort symptoms to come on and sometimes longer. The adrenaline rush allows the individual not to experience the physical symptoms, which is why individuals think they're fine when they are not. Ignoring signs increases the risk of permanent injury. A herniated disc, for example, left untreated, can lead to permanent nerve damage. Chiropractic treatment for rear-end collisions is one of the most effective options available. A chiropractor manipulates the spine to realign the spinal cord, allowing the body to decrease inflammatory cytokine production, which reduces the inflammatory response. Specific techniques and various tools can realign individual vertebrae, restore joint flexibility, and break up the scar tissue so the areas can heal faster. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Chen, Feng, et al. "Investigation on the Injury Severity of Drivers in Rear-End Collisions Between Cars Using a Random Parameters Bivariate Ordered Probit Model." International journal of environmental research and public health vol. 16,14 2632. 23 Jul. 2019, doi:10.3390/ijerph16142632 Davis, C G. "Rear-end impacts: vehicle and occupant response." Journal of manipulative and physiological therapeutics vol. 21,9 (1998): 629-39. Dies, Stephen, and J Walter Strapp. "Chiropractic treatment of patients in motor vehicle accidents: a statistical analysis." The Journal of the Canadian Chiropractic Association vol. 36,3 (1992): 139–145. Garmoe, W. "Rear-end collisions." Archives of physical medicine and rehabilitation vol. 79,8 (1998): 1024-5. doi:10.1016/s0003-9993(98)90106-x
Back injuries from vehicle collisions vary from person to person. Common injuries may include strains, sprains, herniated discs, and fractures, and individuals dealing with certain spinal conditions like spinal stenosis may cause the medical condition to accelerate. Still, the force and physical impact the body absorbs during a crash, no matter how minor the accident or how safe the car is, will cause bodily aches and pains with the potential for other spinal conditions. Chiropractic care, massage, decompression, and traction therapy can relieve symptoms and restore mobility and function. Back Injuries From Vehicle Collisions Depending on how the impact affects the spine, problems can present in various areas of the back. The violent motion can sprain, strain, and fracture spinal components. Even minor incidents can impact mobility. Symptoms can stem from inflammation, compressed nerves, or fractures. Any damage can have long-lasting effects on the vertebrae, nerve roots, and back muscles. A vehicle collision can affect the following: - Lumbar vertebrae - lower back
- Thoracic vertebrae - middle/upper back
- Cervical vertebrae - neck
Each area consists of bones, tissues, muscles, nerves, tendons, and ligaments extending from the neck to the pelvis. - The most common back injuries are to the neck and lower back, where the most movement and shifting occurs, often causing nerve damage.
- The central placement and rigid structure make middle back injuries less common.
- Upper back injuries that connect the rib and chest region can affect breathing.
- Soft tissue injuries might not show up immediately.
Symptoms After a vehicle collision, it's common to feel sore all over. The symptoms can range from manageable discomfort to complete immobility. Individuals may experience the following: Muscle spasms - The muscle may repeatedly twitch, feel like hard knots, and feel tender to the touch.
- Muscle spasms can vary in pain levels from mild to debilitating.
Stiffness - Individuals may not feel as flexible because of the muscle tension that activated during the crash to protect the body.
- Stiffness can go away after light stretching or continue throughout the day.
Burning or Shooting Pain - A burning or shooting pain may travel down the back and buttocks through the back of one or both legs.
- It can be mild, dull aches and pains that go away quickly or last for days.
- Changing positions, such as sitting up after waking up or standing up after sitting, can cause sharp acute pain.
- Facet disease may cause neck or shoulder pain.
Discomfort When Walking or Standing - Certain physical activities can cause a throbbing sensation or mild pain when attempting to perform various tasks.
Tingling and/or Numbness - Tense muscles can pinch nerves leading to sensations of tingling or numbness in the legs, feet, arms, or hands.
Head Issues - Headaches, dizziness, or disorientation can present.
Spinal Disorders Back injuries from vehicle collisions can result in a degenerative disc disorder months or years later. It can also speed up health issues individuals didn't know they had before the crash. As the body ages, previous damage combined with degeneration can result in: - Pinched nerves
- Sciatica
- Bulging discs
- Herniated discs
- Spinal stenosis
- Degenerative disc disease
- Foraminal stenosis
- Spondylolisthesis
- Spinal osteoarthritis
- Bone spurs
- Degenerative scoliosis
Discogenic pain - Damage to spinal discs causes discogenic pain, often sharp impulses or shooting sensations.
- Individuals can experience symptoms in different ways:
- Some individuals feel better when standing, sitting, or lying down, while the positions or motions worsen the symptoms for others.
Chiropractic Care and Therapies Chiropractic treatment can rule out critical issues and expedite recovery time. Benefits include: Pain Symptom Relief - Chiropractic relieves pain in the affected areas and throughout the body.
- Massaging and decompression release endorphins.
Inflammation Alleviation - Micro-tears within the muscles and ligaments are common and cannot be found through a standard x-ray.
- Spinal adjustments can bring the spine back into alignment, producing natural anti-inflammatory properties to assist with discomfort and heal the tears.
Scar Tissue Breakdown - Muscles can get scarred, causing stiffness and soreness.
- Chiropractic massage targets these areas and breaks down the build-up quicker than if it was left to heal on its own.
- Less scar tissue means faster recovery.
Range of Motion and Mobility Restored - Back injuries can result in restricted mobility.
- It may be difficult to turn or move when the muscles are inflamed.
- Mobilizing the spine through adjustments restores the proper range of motion.
Decreased Medication Use - Prescription pain medications can turn into dependency.
- Chiropractic adjustments can ensure that the injury is healed and the pain is not just masked.
Long-Term Benefits - Receiving chiropractic care can help prevent minor injuries from worsening into serious and chronic conditions.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make your own healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Erbulut, Deniz U. "Biomechanics of neck injuries resulting from rear-end vehicle collisions." Turkish neurosurgery vol. 24,4 (2014): 466-70. doi:10.5137/1019-5149.JTN.9218-13.1 National Spinal Cord Injury Statistical Center. (2020) "Spinal Cord Injury: Facts and Figures at a Glance." https://www.nspine injurysc.uab.edu/Public/Facts%20and%20Figures%202020.pdf Rao, Raj D et al. "Occupant and Crash Characteristics of Elderly Subjects With Thoracic and Lumbar Spine Injuries After Motor Vehicle Collisions." Spine vol. 41,1 (2016): 32-8. doi:10.1097/BRS.0000000000001079 Rao, Raj D et al. "Occupant and crash characteristics in thoracic and lumbar spine injuries resulting from motor vehicle collisions." The spine journal: official journal of the North American Spine Society vol. 14,10 (2014): 2355-65. doi:10.1016/j.spinee.2014.01.038
The thoracic spine, also known as the upper or middle back, is designed for stability to anchor the rib cage and protect the organs in the chest. It is highly resistant to injury and pain. However, when thoracic back pain does present, it is usually from long-term posture problems or an injury. Thoracic back pain is less common than lower back and neck pain, but it does affect up to 20% of the population, particularly women. Treatment options include chiropractic for quick and long-term pain relief. Thoracic Back Pain and Soreness The thoracic area is vital for various functions related to: Common reasons for experiencing thoracic back pain include: - A direct hit or high-impact injury from a fall.
- Sports injury.
- Automobile accident.
- Unhealthy postures that put the spine in chronic misalignment, causing strain.
- Repetitive overuse injury from bending, reaching, lifting, twisting.
- Poor core or shoulder mechanics, causing muscle imbalance.
- Muscular irritation, the large upper back muscles are prone to developing strains or tightness that can be painful and difficult to alleviate.
- De-conditioning or lack of strength.
- Joint dysfunction can come from a sudden injury or natural degeneration from aging. Examples include facet joint cartilage tear or joint capsule tear.
Upper back pain usually feels like a sharp, burning pain localized to one spot or a general achiness that can flare up and spread out to the shoulder, neck, and arms. Types of Upper Back Pain These include: - Myofascial pain
- Spine degeneration
- Joint dysfunction
- Nerve dysfunction
- General spinal misalignments
Depending on what specific tissues are affected, pain can occur with breathing or arm use. It is recommended to have a healthcare professional perform an examination and get an accurate diagnosis. A chiropractor understands the delicate balance and functions that the thoracic spine provides and can develop a proper treatment plan. Chiropractic Treatment options will depend on the symptoms, underlying dysfunctions, and individual preferences. Recommendations for treatment often include: - Spine adjustments to improve alignment and nerve integrity.
- Posture training to maintain spinal alignment.
- Therapeutic massage.
- Exercise training to restore muscular balance.
- Non-invasive pain-relieving techniques.
- Health coaching.
Plant-Based Diets for Weight Loss Individuals who follow vegan, vegetarian, and semivegetarian diets have reported and shown they are less likely to be overweight or obese. This can indicate that reducing intake of meat and animal products is beneficial for weight loss. Studies have found that individuals who follow a vegan diet may lose more weight than individuals on a more conventional weight loss diet, even with similar calories consumed, and often have significant improvements in blood sugar and inflammation markers. Plant-Based Protein and Muscle Gain Some plant-based proteins are just as effective as animal protein at promoting muscle gain. A study found that supplementing rice protein following resistance training had similar benefits to whey protein supplementation. Both groups had: General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Briggs AM, Smith AJ, Straker LM, Bragge P. Thoracic spine pain in the general population: prevalence, incidence and associated factors in children, adolescents and adults. A systematic review. BMC Musculoskelet Disord. 2009;10:77. Cichoń, Dorota et al. “Efficacy of Physiotherapy in Reducing Back Pain and Improve Joint Mobility in Older Women.” Ortopedia, traumatologia, rehabilitacja vol. 21,1 (2019): 45-55. doi:10.5604/01.3001.0013.1115 Fouquet N, Bodin J, Descatha A, et al. Prevalence of thoracic spine pain in a surveillance network. Occup Med (Lond). 2015;65(2):122-5. Jäger, Ralf et al. “Comparison of rice and whey protein isolate digestion rate and amino acid absorption.” Journal of the International Society of Sports Nutrition vol. 10,Suppl 1 P12. 6 Dec. 2013, doi:10.1186/1550-2783-10-S1-P12 Joy, Jordan M et al. “The effects of 8 weeks of whey or rice protein supplementation on body composition and exercise performance.” Nutrition journal vol. 12 86. 20 Jun. 2013, doi:10.1186/1475-2891-12-86 Medawar, Evelyn et al. “The effects of plant-based diets on the body and the brain: a systematic review.” Translational psychiatry vol. 9,1 226. 12 Sep. 2019, doi:10.1038/s41398-019-0552-0 Newby, PK et al. “Risk of overweight and obesity among semivegetarian, lactovegetarian, and vegan women.” The American journal of clinical nutrition vol. 81,6 (2005): 1267-74. doi:10.1093/ajcn/81.6.1267 Pope, Malcolm H et al. “Spine ergonomics.” Annual review of biomedical engineering vol. 4 (2002): 49-68. doi:10.1146/annurev.bioeng.4.092101.122107
Teenagers just like adults can experience back pain from accidents, sports injuries, a sedentary lifestyle, part-time jobs, chores, etc. However, sitting too long in school along with heavy backpacks can also contribute to compromised spinal health. Poor spinal health in adolescence can lead to chronic pain in adulthood. Chiropractic professionals can help these young individuals address and prevent spinal issues/injuries to maintain a healthy spine. Teenagers Spine Issues If discomfort or pain presents many just push through, as they and their spines are young. There are common spinal dysfunctions that teens and parents should be aware of, these include: Disc injuries Teenagers can put a serious strain on the spine from various forms of physical activity, jumping, dancing, and playing. This pressure gets transmitted through the spine. During a teenager's development, this can result in permanent disc damage. Scoliosis A spinal deformity or exaggerated curvature of the spine is common and affects young children and teens. It usually happens during the growth spurt just before puberty. This is why it is important to have a teenager’s spine checked regularly and analyzed for signs/symptoms of scoliosis. Spondylolysis This condition is often associated with sports injuries. It happens when teenagers overextend/overreach their backs. It’s most common in gymnastics, weight lifting, tennis, football, diving, and other similar sports. Protection and Prevention There are several ways that parents and healthcare providers can help teenagers make healthy decisions to achieve and maintain optimal spinal health. Sitting less, moving more Children are taught to sit from a very young age. In school, watching t.v., or doing homework, teenagers spend more time sitting than their bodies should. Teenagers need to stand, walk and move around just like adults to protect their spines from degeneration and injury. Maintaining healthy posture Teens that learn how to maintain proper posture at a young age are better able to maintain it for the rest of their life. Learning proper posture at a young age. Sports safety Playing sports is healthy. However, there is a risk associated with teen sports. Although they are taught to play safely, encourage them to continue to educate themselves about sports injuries and know how to address them. Chiropractic Support At Injury Medical Chiropractic and Functional Medicine Clinic, we’re committed to helping young adults and adolescents overcome and prevent spinal injuries that could turn into chronic pain conditions. We are continually developing our chiropractic and physical therapy treatment approaches to achieve optimal results. Sleep and Growth Hormone In Children Growth is primarily controlled by growth hormones. This hormone is regulated by the hypothalamus and the pituitary gland. Sleep plays an important role in the proper function of these glands. A review showed that: - Growth hormone levels rise and peak at the onset of deep sleep
- Multiple but smaller peaks were seen during other sleep stages
- Individuals that have a delay in the onset of deep sleep have delayed peaks in growth hormone levels
For children to grow properly, they need to have adequate levels of growth hormone. This means they need to have a sufficient amount of sleep. The proper amount of sleep is vital for healthy body composition. A study measured the body composition of preschool-aged children. The study found that children that had proper levels of sleep had less overall fat mass and reduced body fat. Children and teenagers need to get the proper amounts of sleep for their bodies to grow healthily. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Clement, R Carter et al. “What are normal radiographic spine and shoulder balance parameters among adolescent patients?.” Spine deformity vol. 8,4 (2020): 621-627. doi:10.1007/s43390-020-00074-9 Driehuis, Femke et al. “Spinal manual therapy in infants, children and adolescents: A systematic review and meta-analysis on treatment indication, technique, and outcomes.” PloS one vol. 14,6 e0218940. 25 Jun. 2019, doi:10.1371/journal.pone.0218940 Manansala, Christian et al. “Change in young people's spine pain following chiropractic care at a publicly funded healthcare facility in Canada.” Complementary therapies in clinical practice vol. 35 (2019): 301-307. doi:10.1016/j.ctcp.2019.03.013
As individuals advance in age, the risk of falling starts to become a regular concern. An average of one in four adults over 65 suffers from a fall every year. Around twenty percent of falling accidents result in serious injury. However, experiencing one fall increases the risk of future falls significantly. The most common injuries sustained include: These injuries usually necessitate hospitalization. Therefore minimizing the risks is important for increasing/enhancing an individual's quality of life and help minimize the financial burdens that can come with these types of accidents. Risk Factors for Falling Various factors can determine an increased risk of falling. If there are two or more at the same time, the risk goes up significantly. These factors include: - Poor or improper walking gait mechanics
- Poor balance
- Vision impairment
- Low endurance
- Weakened muscle strength
- Sedentary lifestyle
- Blood pressure issues like hypotension
- Dizziness from certain movements like lying down to sitting/standing
- Medication side effects that cause brain fog, dizziness, sleepiness, etc
- Poor health/underlying conditions
- Anxiety and/or fear of falling
Reducing The Risk/s There are simple ways to reduce risk while optimizing the body's health and vitality. These include: - Discussing health concerns with a doctor and/or chiropractor
- Review medications with doctor or pharmacist, specifically those that cause sleepiness or dizziness
- Exercise regimen
- Balance exercises
- Core strengthening exercises
- A physical therapist or chiropractor can assess the home for safety and possible tripping hazards
- Regular vision check-ups at least every two years
Spinal Health Restoring balance to the body will make the biggest difference in increasing overall health. However, pain, stiffness, and poor health can make getting started a difficult challenge. With the right chiropractic and physical therapy team, getting started does not have to be as challenging, with the transition being made as easily and as smooth as possible. An essential building block for overall optimal health begins with spinal alignment. When the spine is misaligned it can lead to poor nerve circulation/energy. This slows down and interferes with the body's functions. This is often manifested with poor balance, weakness, and pain. Chiropractic spinal alignment addresses whole-body health. A chiropractic practitioner is specialized in non-invasively and systematically restoring not only the alignment of the spine but the entire body. Chiropractic Health Find a chiropractor and talk to them about any health concerns, including falls. A customized chiropractic adjustment treatment plan will be developed along with a fitness and stretching regimen, and dietary adjustments will significantly optimize health and help prevent falls. Dr. Alex Jimenez’s Blog Post Disclaimer The scope of our information is limited to chiropractic, musculoskeletal, physical medicines, wellness, and sensitive health issues and/or functional medicine articles, topics, and discussions. We use functional health & wellness protocols to treat and support care for injuries or disorders of the musculoskeletal system. Our posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate and support directly or indirectly our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. We understand that we cover matters that require an additional explanation as to how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. The provider(s) Licensed in Texas& New Mexico* References Hawk, Cheryl et al. “Pilot study of the effect of a limited and extended course of chiropractic care on balance, chronic pain, and dizziness in older adults.” Journal of manipulative and physiological therapeutics vol. 32,6 (2009): 438-47. doi:10.1016/j.jmpt.2009.06.008
Whiplash injuries very rarely call for surgery. But with those rare occurrences, that are severe cases, surgery is considered appropriate when neck or shoulder pain worsens. Doctors recommend patients go through 4 to 6 weeks of non-surgical treatment. If there is no improvement or the condition is worsening then a doctor could recommend whiplash surgery as the best option. A spine surgeon will recommend the best procedure for the specific injury. Ask all the questions you have to fully understand the exact process, the outcome, and the recovery time. Surgery is an individual's decision. The surgeon can recommend it, but the patient has the final say. The procedure depends on what area/s the cervical spine is injured/damaged. Disc Herniation Depending on the type of trauma individuals can rupture or herniate the intervertebral disc/s, located between the vertebrae. This can generate constant pain, numbness, and weakness. With cases like this sometimes removal of the disc is necessary. A surgeon will remove all or portion of the damaged disc through a process called a discectomy. After the discectomy, a doctor may have to permanently stabilize the area. This is because the spine becomes unstable and can move in abnormal ways. This increases the risk of a serious neurological injury. Therefore a discectomy is usually followed with a re-stabilization of the spine. Spinal stabilization techniques used: Artificial Disc Replacement Cervical artificial disc replacement also known as ADR could be performed instead of standard discectomy combined with spinal fusion. An artificial disc is implanted into the empty space following the procedure. Artificial disc replacement preserves or restores movement of the neck. Fusion and Spinal Instrumentation This form of spine stabilization can be done on its own or in combination with decompression surgery. The bones in the spine fuse together over time usually several months or longer depending on how the surgeon set up the fusion process. The surgeon will use a bone graft or a biological chemical that stimulates bone growth. A surgeon could use spinal instrumentation. These are: - Interbody device/s
- Screws
- Rods
- Plates
These all are used to increase stability and help fuse the bones properly. The fusion prohibits movement between the vertebrae for long-term stability. Stenosis Whiplash surgery could also be necessary if the injury caused the spinal canal in the neck to narrow. Here a cervical corpectomy could be performed to remove part of the vertebra and intervertebral disc/s. This reduces the added pressure on the spinal cord and nerves. A surgeon could also do a laminectomy or a laminoplasty. Both focus on the lamina, which is the bony plate at the back of each vertebra. The lamina protects the spinal cord and canal. The lamina could also present added pressure on the spinal cord. This is where the surgeon will create extra space for the cord by removing all or part of the lamina. This is a laminectomy. A laminoplasty re-shapes the lamina to create more room for the spinal cord. If there is a narrowing of the space where the nerve exits the canal, a cervical foraminotomy could be utilized. The foramen is the area where the nerve roots exit the spinal canal. This is removed to allow for more space for the nerves to move through. A larger pathway is less likely to pinch/compress the nerve. Complications A doctor will discuss all the potential risks before being asked to sign a surgical consent form. Complications can include: - Injury to the spinal cord, nerves, esophagus, carotid artery, vocal cords
- The bone fusion does not heal known as pseudoarthrosis
- Improvement does not occur
- Instrumentation breaks or gets damaged
- Infection
- Bone graft site pain
- Pain and swelling in the leg veins known as phlebitis
- Blood clots in the lung
- Urination problems
Complications could lead to more surgery, so make sure there is a complete understanding of the surgery and the risks before proceeding. The final decision is up to the individual. Whiplash Surgery Recovery After surgery, things might not be great right away. More than likely individuals are out of bed within 24 hours, and on pain meds for 2 to 4 weeks. Individuals will receive instructions on how to sitting down, and standing up. The body needs time to heal, so the doctor will recommend restricting certain activities that involve moving the neck too much. Avoid sports, twisting, or heavy lifting during recovery. And report any problems like fever increased pain, or infection right away. Dr. Alex Jimenez’s Blog Post Disclaimer The scope of our information is limited to chiropractic, musculoskeletal, physical medicines, wellness, and sensitive health issues and/or functional medicine articles, topics, and discussions. We use functional health & wellness protocols to treat and support care for injuries or disorders of the musculoskeletal system. Our posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate and support directly or indirectly our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. We understand that we cover matters that require an additional explanation as to how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. The provider(s) Licensed in Texas& New Mexico*
Minimally invasive spine surgery known as M.I.S.S is an option to traditional open surgical procedures, as well as an alternative when non-surgical approaches are working but the pain or condition is becoming worse, regardless. These are performed to treat a variety of spinal disorders like: - Bone spurs
- Degenerative disc disease
- Herniated disc
- Scoliosis
- Spinal instability
- Spinal stenosis
- Spinal tumors
Minimally invasive surgery can offer potential benefits. These include - A small/tiny incision/s
- Minimal cutting through soft tissues like ligaments, and muscles
- Outpatient option/s
- Reduced post-operative pain
- Quicker recovery
The Focus of Spine Surgery There are two main goals when it comes to spine surgery or rather the goal/focus of the surgery. These are decompressing and stabilizing the spine. Decompression of the spine Spinal decompression involves removing any tissue/s that are compressing/pinching the nerve structures like a spinal nerve root or the spinal cord itself. Bone spurs and fragments from a herniated disc are the types of tissue/s that can cause neural compression. Stabilization of the spine An abnormal movement of one or more levels/segments of the spinal cord can cause back pain, neck pain, or both. Surgeries that are meant to stabilize and stop these abnormal movements utilize spine instrumentation combined with fusion. Spine Surgery Techniques Minimally invasive spine surgery techniques include: - Percutaneous or through the skin
- Mini-open or small incision procedure/s
Rather than cutting through soft tissues, a tubular retraction instrument generates a tunnel that expands and passes between the muscle/s to access the spine's column. Then an endoscope or a tiny video camera goes in and around the area, projecting a visualization of what's happening on a monitor during the procedure. This is the surgeon's/team's eyes as they work to repair the damage. The surgery is run through the tubular retraction system along with any specially designed instruments that are needed. Types of surgical procedures performed with minimally invasive surgery include: - Discectomy
- Microdiscectomy
- Foraminotomy
- Microforaminotomy
- Microlaminectomy
- Microlaminotomy
The micro means that the surgery is done using a special microscopic camera to view the disc/s and nerve/s. Imaging scans, systems, and image-guidance technologies, like fluoroscopy, which is a real-time x-ray are utilized during the surgery pinpointing the key aspects of the patient’s spinal anatomy. The surgical imaging shows 2D and 3D views, which guides the placement of any instrumentation, like pedicle screws. Disorders Treated with Minimally Invasive Surgery Degenerative disc disease Degenerative disc disease is known as DDD often develops progressively in older adults and affects the intervertebral discs. The normal wear and tear of cellular age-related changes in the body can cause the spine's discs to: - Stiffen
- Lose Flexibility
- Loss of Strength
- Loss of Height
- Lose shape, along with the ability to absorb/distribute the forces associated with moving
These structural changes increase the risk of disc herniation and subluxations. Herniated discs A herniated disc also called a slipped, bulging, and ruptured disc. This happens when the soft gel cushion of a disc breaks through the protective outer layer. Other than the damaged disc, the loose interior gel can also irritate and inflame the nerves causing back pain. Scoliosis Scoliosis is an abnormal sideways curve of the spine that can cause progressive spinal deformity. A scoliotic curve can look like an “S” or “C.” Most cases have no known cause, and while the condition is more commonly associated with children, adults can develop scoliosis, as well. Spinal stenosis Spinal stenosis happens when the spinal nerve roots and the spinal cord become compressed/pinched. These nerves branch off the spinal cord and exit the spinal canal through passageways called neuroforamen. Nerve and spinal cord compression can cause symptoms like: - Pain
- Weakness
- Tingling sensations
- Numbness
- Sometimes, pain can travel into the arms or legs
Spine Surgery Risks With any spine surgery there are potential risks and complications that can occur. Here are some possible complications that can happen during and after surgery, with both open and minimally invasive procedures. Candidate for Surgery Minimally invasive spine surgery does offer many benefits: - Tiny incision
- Less pain
- Reduced risk
- Faster recovery
Let's not forget that M.I.S.S is still surgery. Less than 5% of people with back or neck pain need spine surgery and, surgery is the last resort for treating pain and symptoms caused by a spinal condition/disorder. It is only when non-surgical treatments like chiropractic, acupuncture, physical therapy, medication, or spinal injections do not reduce symptoms in 3 to 6 months. This is when you qualify to be a candidate for spine surgery. There are certain types of spinal disorders that require urgent or immediate surgical intervention. Talk with your doctor, chiropractor, or spine specialist about the pain, the symptoms, and compare the results of the different therapies/treatments and go from there. With any type of surgery there are many considerations to discuss before making a decision to treat back or neck pain and if minimally invasive surgery could be an option.
A Burst Fracture A burst fracture describes an injury to the spine where the vertebrae get compressed severely. These types of injuries occur from severe trauma, like an automobile accident or a serious fall, sports injury, work injury. These injuries entail a great deal of force into the spine, so much so that a vertebra can get crushed. When crushed in the front of the spine, a wedge-shaped fracture occurs and is known as a compression fracture. But if the vertebral body gets crushed in all directions this is known as a burst fracture. The term burst means that the vertebral body spreads out in all directions. Severe Injury This is a much more severe injury than a compression fracture. With the bones crushed and possible rough jagged edges, if they spread out the spinal cord has a high probability of being injured. The fragments can bruise the spinal cord causing paralysis or partial neurologic injury. The spine becomes far less stable than from a compression fracture. Nerve Injury Neurologic injuries from a burst fracture can range from no injury to paralysis. This depends on the amount of force present at the time of the injury and how much the spinal canal is compromised. - A greater amount of force equals more bony fragments that can be forced into the spinal canal and cause higher loss of spinal cord function.
This can cause loss of: - Strength
- Sensation
- Reflexes below the injury
With an incomplete spinal cord injury, partial paralysis or partial reflex loss occurs. With a mild burst fracture, only short-term symptoms could be present and no neurologic injury. Intense Pain Burst fractures can cause intense pain and the pain is right where the trauma took place. But pain can also present in the legs and feet depending on how the spinal nerves were affected, shifted or pinched. Patients complain of an electric tingling or shooting type sensation in their legs with spinal cord compression. With a burst fracture, individuals are unable to walk right after the trauma. But the pain percentage present is severe enough that they know not to try and walk. Diagnosis If at the sight of the accident the patient says that they have severe back pain should not be in a seated flexed position. They need to be kept lying flat and transported in a flat position. If they stand or sit with a burst fracture, it can increase the possibility of a neurologic injury. Burst fractures require immediate medical attention from an orthopedic or neurosurgeon. The patient is taken to an emergency room and x-rays, CT scans are gathered. The diagnosis of a burst fracture is typically made with x-rays and a CT scan. Sometimes, an MRI will be ordered to assess the amount of: - Soft tissue trauma
- Bleeding
- Ligament injury
The CT scan and x-rays allow the doctor to determine the level of the fracture, and if it is a: - Compression fracture
- Burst fracture
- Fracture-dislocation
This will determine how much the spinal canal has been compromised and if its angulation or angle has taken an abnormal bend or curve. These factors all contribute to the development of an optimal treatment plan. The physical exam will document: - Spinal deformity and Angulation of the spine
- Tenderness of the spine where the fracture is located
- Neurologic exam
Neurologic exam should include testing: - Muscle strength
- Sensation
- Reflexes of the lower extremities
- Testing of bowel and bladder control
Treatment & Recovery A stable burst fracture can be treated without surgery. A stable burst fracture falls into these parameters: - There is no neurologic injury
- The angulation is less than 20 degrees
- The amount of spinal canal compromise is less than 50%
With this type of treatment, a brace along with physical therapy/chiropractic can have excellent results. A turtle or clamshell brace TLSO (Thoracic Lumbar Sacral Orthosis) is a body cast used in the treatment of a burst fracture. The brace is worn for eight to twelve weeks for adequate and optimal healing. There are times when a fracture thought stable and treated can start to angulate. This may require surgery. However, all burst fractures require some form of treatment. Recovery - Nonsurgical treatment patients stay in the hospital for one or two days while their brace is fit.
- X-rays are done in the standing position to make sure the spine stays stable.
- Pain medications are prescribed for three to four weeks
- Non-narcotic medications can begin after the final week
When the brace is removed, physical therapy and chiropractic are instituted to help return strength to the core and lower extremities. Surgical patients will remain in the hospital for three to five days. - They will be fitted with a brace after the incisions present less pain and are recovered from the surgery.
- They can walk within one or two days with the help of a physical therapist.
- X-rays are taken to follow the position of the spine and see how the healing is progressing.
- Chiropractic/Physical therapy is implemented to help with core strength and lower extremity strength.
Recovery time depends on the severity of the neurologic injury. - Patients that don't have a neurologic injury can make a full recovery with return to most activities.
- Patients with partial neurological injuries can also expect to fully recover.
- Unfortunately, with permanent neurologic injury, recovery can be limited.
But treatment for burst fractures today is superior to what they were years ago, especially with spine specialists and specific spinal procedures. Chiropractic Rehab Chiropractic is not a treatment for fractures but is a treatment for subluxations and rehabilitation with these types of fractures. Once a fracture has stabilized and healed properly, a chiropractic evaluation can rule out any lingering subluxation, herniation, and joint restriction. The adjustments are safe and effective in establishing optimal function to a subluxated joint. We focus on what works for you. We also strive to create fitness and better the body through researched methods and total wellness programs. These programs are natural and use the body’s own ability to achieve goals of improvement.
Title: Conservative care and axial distraction therapy for the management of cervical and lumbar disc herniations and ligament laxity post motor vehicle collision.
Dr. Alex Jimenez, doctor of chiropractic, focuses on the diagnosis, treatment and prevention of a variety of injuries and conditions associated with the musculoskeletal and nervous systems, utilizing several chiropractic methods and techniques. The following procedures may be similar to his own but can differ according to the specific issue and complications by which the individual is diagnosed.
Abstract: This middle-aged female was injured in a vehicle collision causing her to sustain disc and additional ligament injuries in the cervical and lumbar spine. Diagnostic studies included physical examination, orthopedic and neurological testing, lumbar MRI, multiple cervical MRI’s, CRMA with motion cervical radiographs and EMG studies. Typically, conservative care is initiated prior to interventional procedures, and this case study seeks to explore the usage of passive therapy for mechanical spine pain and noted anatomic disc lesions after failure of interventional procedures. She reported both short term and long term success regarding pain reduction along with improvement in her activities of daily living after initiating conservative care, and continued to report further reductions in pain with periodic pain management using conservative care.
Automobile accidents are often unpredictable circumstances which can involve many complications. Whether it’s a minor or severe collision, many individuals are forced to deal with all the implications that come after being involved in an auto accident on their own, a frustrating process that frequently ends with victims being on the losing end of their benefits. Injured and without a car, approaching the best course of action following an auto accident doesn’t need to be a difficult circumstance and we know the best procedures to help you recover from your situation. According to the National Highway Traffic Safety Administration (NHTSA), approximately 2.6 million individuals are injured each year in automobile accidents, accounting for 95 percent of all injury causing accidents on the roads. During a car crash, the sudden force of the impact can commonly cause subluxations or spinal misalignments in the body, a condition where the complex structures surrounding the spine are affected, distorting the normal alignment of the vertebra, irritating nerves, ligaments, and discs, overall affecting their natural function and your health.
The majority of people who suffer a whiplash type injury as a result of an automobile accident are instructed to wear a neck brace but, an abundant amount of research suggests that neck braces, also known as cervical collars, may actually cause more harm than good. A new study shows that individuals who experienced whiplash have a better chance of recovering from their injury and symptoms without the use of a cervical collar. In addition, these findings, together with previous studies, also suggest that individuals may have better recovery results with active treatments such as chiropractic care and exercise. Other studies have also demonstrated that the use of cervical collars can prolong pain and disability in individuals with whiplash injuries. A 2008 meta-analysis of recent studies on whiplash treatment found that cervical collars are fundamentally meant to be used in cases of spinal fractures for it to be beneficial. It’s use in other types of injuries or conditions can actually prevent recovery. The function of cervical collars is to immobilize the spine in order to prevent further damage or injury. Nonetheless, the neck’s inactivity resulting from the use of cervical collars can eventually cause muscle degeneration and decreased function. Chiropractic care for treating this type of injury includes neck adjustments and manual manipulation, followed by gentle stretches and exercises to help speed up the rehabilitation process. By re-aligning the cervical spine and correcting tissue damage as a result of the injury, a chiropractor can help restore the affected individual’s normal mobility and decrease their pain and other symptoms.
Whiplash refers to a soft-tissue injury of the cervical spine, or neck, caused by a strong, abrupt, back-and- forth movement of the head, typically caused by an automobile accident, although this type of injury can also be the result of a sports accident or other trauma. Several studies suggest that up to 43% of individuals generally suffer from long-term symptoms following a whiplash injury. Further studies also suggest that of those individuals whom still experience symptoms after three months of the injury, almost 90% of the time, they will develop chronic whiplash symptoms. Although conventional treatment can be used to treat whiplash, chiropractic treatment is notably recommended to treat many automobile accident injuries and the improvement results are quite significant, according to research. The authors of a study researched the effectiveness of chiropractic treatment in 28 individuals who had been previously diagnosed with chronic whiplash pain and other symptoms. Each person had been referred to a chiropractor in between a range of 3 months to almost 4 years after their accident, with an average of 15.5 months. After following the appropriate chiropractic treatment, 26 of the affected individuals, in other words, 93% of the people with chronic whiplash symptoms, had improved considerably: 16 individuals had improved by one symptom group while 10 individuals had improved by two symptom groups. For whiplash, a chiropractor often uses spinal adjustments and manual manipulations to correct cervical spine misalignments in order to minimize the stress and tension on the surrounding neck muscles. Chiropractic treatment can also include a set of stretches or exercises to continue rehabilitating whiplash symptoms.
|
Automobile accidents are emotionally and physically traumatic events. After an accident, individuals assume that they are okay if they don't have any broken bones or gashing cuts. However, even minor accidents can lead to significant damage, but the individual doesn't know it. An invisible/delayed injury is any injury that is not immediately obvious or is not experienced by the individual until hours, days, or weeks later. The most common are soft tissue injuries, back injuries, whiplash, concussions, and internal bleeding. This is why it is imperative to see a doctor or chiropractic accident specialist as soon as possible after an accident. Invisible Injuries Auto Accidents The body goes into a fight or flight mode in a vehicle accident. That means a massive adrenaline surge makes anything happening to the body go unnoticed and unfelt. The individual does not feel pain and discomfort symptoms until later or much later. Soft Tissue - A soft tissue injury affects muscles, tendons, ligaments, and body parts other than bone.
- Even at low speeds, accidents, and collisions generate a significant force on the body.
- Drivers and passengers often come to a sudden stop along with the vehicle or get thrown around.
- This places intense stress on joints and other areas of the body.
Whiplash The most common invisible soft-tissue injury is whiplash. - Where the neck muscles are suddenly and forcefully thrown forward and then back, causing the muscles and ligaments to stretch beyond their normal range of motion.
- The injury typically results in pain, swelling, reduced mobility, and headaches.
- Symptoms may not present right away.
- Left untreated, whiplash can lead to long-term chronic pain.
Head Injuries - Head injuries are another common invisible injury.
- Even if the head did not hit/impact anything, the force and momentum can cause the brain to collide with the inside of the skull.
- This can lead to a concussion or even more serious brain injuries.
Concussion A concussion is a traumatic brain injury. Individuals can have a concussion without losing consciousness, depending on the accident's severity. Symptoms may be delayed or not experienced, but delayed treatment can lead to a longer recovery. Symptoms can include: - Fatigue.
- Headache.
- Confusion.
- Inability to remember the accident.
- Nausea.
- Ringing in the ears.
- Dizziness.
Back Muscles or Spine Injuries Back muscles and spinal cord injuries are invisible injuries that can happen after an automobile accident. Signs of a back injury include: - The back muscles can be strained due to the impact and tension build-up.
- Sore muscles or pain may not present until a day or two later.
- Body stiffness.
- Reduced mobility.
- Muscle spasms.
- Trouble walking, standing, or sitting.
- Headaches.
- Numbness and tingling.
Injuries to the spine, even serious ones, may not be apparent immediately. - The impact can cause the spine to shift out of alignment profoundly.
- Swelling and bleeding in or around the spinal cord can cause numbness or paralysis that can gradually progress.
- This invisible injury can have long-term consequences, including paralysis.
Chiropractic Care Chiropractic is an effective treatment for neuromusculoskeletal injuries. The chiropractor will assess the damage and its severity to determine the best treatment for the individual. It relieves pain and discomfort symptoms, loosens and relaxes the muscles, and restores alignment, mobility, and a full range of motion. Chiropractic uses several tools and techniques to restore the spine and body balance. Results include: - Pain relieved.
- Improved circulation.
- Restored alignment.
- Released compressed/pinched nerves.
- Improved posture and balance.
- Improved flexibility.
- Restored mobility.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References “Automobile-related injuries.” JAMA vol. 249,23 (1983): 3216-22. doi:10.1001/jama.1983.03330470056034 Barach, P, and E Richter. “Injury prevention.” The New England Journal of Medicine vol. 338,2 (1998): 132-3; author reply 133. doi:10.1056/NEJM199801083380215 Binder, Allan I. “Neck pain.” BMJ clinical evidence vol. 2008 1103. 4 Aug. 2008 Duncan, G J, and R Meals. “One hundred years of automobile-induced orthopedic injuries.” Orthopedics vol. 18,2 (1995): 165-70. doi:10.3928/0147-7447-19950201-15 “Motor Vehicle Safety.” Annals of emergency medicine vol. 68,1 (2016): 146-7. doi:10.1016/j.annemergmed.2016.04.045 Sims, J K et al. “Automobile accident occupant injuries.” JACEP vol. 5,10 (1976): 796-808. doi:10.1016/s0361-1124(76)80313-9 Vassiliou, Timon, et al. “Physical therapy and active exercises--an adequate treatment for prevention of late whiplash syndrome? Randomized controlled trial in 200 patients.” Pain vol. 124,1-2 (2006): 69-76. doi:10.1016/j.pain.2006.03.017
Whiplash-associated disorders, or WAD, describe injuries sustained from sudden acceleration/deceleration movements. It is a common outcome after a motor vehicle collision but can also be caused by sports injuries, falls, or assaults. Whiplash refers to the mechanism of the injury, while WAD refers to the presence of symptoms like pain, stiffness, muscle spasm, and headaches. A WAD prognosis is unpredictable, with some cases remaining acute with a full recovery, while others progress to chronic conditions with long-term symptoms and disability. Early intervention recommendations include rest, chiropractic care and physical rehabilitation, massaging and stretching exercises, and an anti-inflammatory diet. Whiplash Associated Disorders Cervical hyperextension injuries happen to drivers and passengers of moving, slow-moving (less than 14 miles per hour), and stationary vehicles when struck from behind. - The individual's body is thrown forward, but the head does not follow the body and instead whips forward, resulting in hyperflexion or extreme forward movement of the neck.
- The chin limits forward flexion, but the momentum can be sufficient to cause cervical distraction and neurological injuries.
- When the head and neck have reached maximum flexion, the neck snaps back, resulting in hyperextension or extreme backward movement of the neck.
Pathology Most WADs are considered soft tissue-based injuries with no fractures. Stages The injury goes through stages: Stage 1 - The upper and lower spine experiences flexion in stage one.
Stage 2 - The spine takes on an S-shape while extending and eventually straightens, causing lordosis.
Stage 3 - The entire spine is hyperextending with an intense force that causes the facet joint capsules to compress.
Symptoms Whiplash-associated disorders can be classified through grades by the severity of symptoms, including neck pain, stiffness, occipital headache, cervical, thoracic, and lumbar back pain, upper-limb pain, and paraesthesia. Grade 0 - No complaints or physical symptoms.
Grade 1 - Neck complaints but no physical symptoms.
Grade 2 - Neck complaints and musculoskeletal symptoms.
Grade 3 - Neck complaints and neurological symptoms.
Grade 4 - Neck complaints and fracture and/or dislocation.
- Most cervical fractures occur predominantly at C2 or C6, or C7.
- Most fatal cervical spine injuries occur at the craniocervical junction C1 or C2.
Affected Spinal Structures Some symptoms are thought to be caused by injury to the following structures: Causes of pain can be from any of these tissues, with the strain of the injury causing secondary edema, hemorrhage, and inflammation. Joints - Zygapophyseal joints
- Atlanto-axial joint
- Atlanto-occipital joint
- Intervertebral discs
- Cartilaginous endplates
Adjacent Joints Ligaments - Alar ligament
- Anterior atlanto-axial ligament
- Anterior atlanto-occipital ligament
- Apical ligament
- Anterior longitudinal ligament
- Transverse ligament of the atlas
Bones - Atlas
- Axis
- Vertebrae C3-C7
Nervous Systems Structures - Nerve roots
- Spinal cord
- Brain
- Sympathetic nervous system
Vascular System Structures - Internal carotid artery
- Vertebral artery
Chiropractic Care A chiropractor will identify areas of restricted joint motion, muscle tension, muscle spasm, intervertebral disc injury, and ligament injury. - They will analyze posture, and spinal alignment, check for tenderness, tightness, and how well the spinal joints move.
- This will allow the chiropractic physical therapy team to understand the injured body mechanics and how the spine is operating to make a thorough diagnosis.
- The doctor will order imaging tests like an x-ray or an MRI to evaluate any degenerative changes that may have existed before the whiplash injury.
- Once the injury has been accurately diagnosed, the chiropractor will design a personalized treatment plan.
Spinal Adjustments - Spinal manipulation is applied to areas of the spine that are out of alignment to realign the spine and activate the healing process.
- Flexion-distraction technique is a gentle technique that uses slower, less intense pushing motions on the discs used to treat disc herniations that often occur after a whiplash injury.
- Instrument-assisted manipulation utilizes special instruments to apply various forces or massage settings to the area.
- Targeted spinal manipulation targets specific areas to rework, release, and rebuild the structures.
- Massage Therapy stimulates the affected muscles to relax them from their tense state.
- A treatment plan may utilize:
- Instrument-assisted therapy
- Trigger point therapy
- Resistance-based stretches to rehabilitate soft tissue damage.
Our chiropractic team is ready to help you feel your best so you can return to normal activities and get on with your life. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Pastakia, Khushnum, and Saravana Kumar. "Acute whiplash associated disorders (WAD)." Open access emergency medicine: OAEM vol. 3 29-32. 27 Apr. 2011, doi:10.2147/OAEM.S17853 Ritchie, C., Ehrlich, C. & Sterling, M. Living with ongoing whiplash-associated disorders: a qualitative study of individual perceptions and experiences. BMC Musculoskelet Disord 18, 531 (2017). https://doi.org/10.1186/s12891-017-1882-9 https://www.sciencedirect.com/topics/medicine-and-dentistry/whiplash-associated-disorder Sterling, Michele. "Whiplash-associated disorder: musculoskeletal pain and related clinical findings." The Journal of manual & manipulative therapy vol. 19,4 (2011): 194-200. doi:10.1179/106698111X13129729551949 Wong, Jessica J et al. "Are manual therapies, passive physical modalities, or acupuncture effective for the management of patients with whiplash-associated disorders or neck pain and associated disorders? An update of the Bone and Joint Decade Task Force on Neck Pain and Its Associated Disorders by the OPTIMa collaboration." The spine journal: official Journal of the North American Spine Society vol. 16,12 (2016): 1598-1630. doi:10.1016/j.spinee.2015.08.024 Woodward, M N et al. "Chiropractic treatment of chronic 'whiplash' injuries." Injury vol. 27,9 (1996): 643-5. doi:10.1016/s0020-1383(96)00096-4
When the body goes through intense trauma like a car, truck, crash, or accident, the trauma can slip, bulge, herniate, or rupture the spinal fluid-filled discs that can extrude from the disc space, causing the nucleus pulposus to tear through the annulus fibrosus and compress the nerve roots causing pain. Depending on the severity and force of the crash or accident, a herniated disc can cause the vertebrae to push into the spinal canal, where it can compress, irritate, and/or injure the spinal cord, which can lead to other health issues. Nerve impingement from a herniated disc can also cause numbness and tingling in the hands, arms, legs, and feet. A chiropractic spine disc herniation decompression treatment plan can heal the herniation, realign the spine, stretch the muscles and joints, and rehabilitate the body back to top form. Spine Disc Herniation Symptoms of Herniation Signs and symptoms depend on the spinal area and whether the disc is rubbing or compressing a nerve. Pain is often described as a sharp or burning sensation. A herniated disc usually affects one side of the body. Pain Presents When Sitting Down - sitting causes a significant strain on the lower spinal discs. When sitting, the pain experienced can worsen. Arm or leg pain - Depending on the herniated disc, pain can spread to other surrounding areas. - For a lower herniation, this could be the buttock, thigh, calf, and foot.
- For a herniated disc in the neck region, pain can be felt in the shoulder and arm.
Pain can present in the arm or leg when coughing, sneezing, or moving into certain positions. Numbness or tingling - presents from the compressed nerves and spreads as the average blood/energy flow is disrupted. Muscle Weakness - the affected nerves that support the spinal muscles can lose normal strength causing awkward postures and fatigue. A herniated disc can be present without symptoms - individuals won't know unless spinal imaging is ordered. Sciatica Sensations - the damaged nerve roots affect the ability to function correctly and can cause burning pain, numbness, weakness, and tingling along the front and/or back of the thigh, leg, and/or foot. This can result from direct compression or chemical irritation from a leaked out herniated disc that causes inflammation around the nerve root area. Chiropractic Injury Care When a disc herniates, it inhibits the body from communicating and healing itself. To activate proper communication from the brain to the rest of the body, chiropractors perform spine disc herniation decompression which clears the neural system and opens the lines of communication. Spine Disc Herniation Decompression Nonsurgical spinal decompression gently stretches the spine to relieve pressure and heal the herniated disc. It is a safe procedure considered a natural alternative compared to surgery or pharmaceutical approaches. Spinal decompression therapy: - It is safe for all ages
- It is non-invasive
- Sessions take between 30 to 45 minutes, depending on the individual and the injury that could require multiple sessions.
- Offers a quicker recovery time
- It is performed on a computer-controlled table customized to the individual's specific needs and injuries.
A treatment plan can expedite the recovery process, rehabilitate and strengthen the whole body, and help avoid minimally invasive spine surgery. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, or licensed physician, and is not medical advice. We encourage you to make your own healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Atlas, Steven J et al. "The impact of disability compensation on long-term treatment outcomes of patients with sciatica due to a lumbar disc herniation." Spine vol. 31,26 (2006): 3061-9. doi:10.1097/01.brs.0000250325.87083.8d Dydyk AM, Ngnitewe Massa R, Mesfin FB. Disc Herniation. [Updated 2022 Jan 18]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK441822/ Gane, Elise M et al. "The Impact of Musculoskeletal Injuries Sustained in Road Traffic Crashes on Work-Related Outcomes: A Systematic Review." International journal of environmental research and public health vol. 18,21 11504. 1 Nov. 2021, doi:10.3390/ijerph182111504 Scuderi, Gaetano J et al. "Symptomatic cervical disc herniation following a motor vehicle collision: return to work comparative study of workers' compensation versus personal injury insurance status." The spine journal: official journal of the North American Spine Society vol. 5,6 (2005): 639-44; discussion 644. doi:10.1016/j.spinee.2005.04.007
A motorcyclist has an increased risk of injury every time they get on their bike and get on the road. There is no barrier to protect them in the case of a crash or accident. Because of this, motorcycle injuries sustained can be life-changing. The most common injuries that motorcycle riders sustain and suffer when involved in accidents and crashes tend to be related to high traffic, speed, distracted drivers, and construction. This means that most common motorcycle accidents and crash injuries are severe. Road Rash Also known as road burn. This is a type of burn that is caused when the body's skin gets badly scraped and shredded from the road. This often happens when a rider is thrown from the motorcycle skidding down the road before coming to a stop. Road rash can happen on any part of the body. For motorcyclists, it is common on the legs, hands, arms, and back. It can be excruciating even though the injury is not considered fatal, complications and overlapping injuries can develop. This is usually in the form of infections that can affect mobility and flexibility issues that can require further medical intervention and rehabilitation. In severe cases, it can require skin grafts. Depending on the severity it can leave permanent scarring. Treatment often includes antibiotics, bandage dressings, burn soothing and disinfectant creams. Fractures and Broken Bones When a motorcycle and a vehicle collide, it is very common for the motorcyclist to get thrown or knocked off with intense force. When the rider hits the ground, the impact alone can cause fractures and breaks. If the rider lands at an awkward angle this can definitely cause a fracture or break. Broken bones can happen anywhere on the body, but are most commonly sustained in the arms and legs. Broken ribs are also common and usually occur when the motorcyclist gets hit or falls hard. Motorcycle endorsement classes emphasize the ATGATT system that stands for All The Gear, All The Time. This means wearing motorcyclist protective clothing and ankle-high boots. Ankle injuries and fractures are commonly sustained from operating a motorcycle. Spinal Cord Injuries If the spinal cord gets injured or damaged the results can be devastating. Depending on the area of the injury, an individual might not be able to walk, use their arms, or move at all. Spinal cord injuries tend to happen when the motorcyclist gets thrown hard or up in the air landing hard on their neck, back, or the body gets pierced by an object. Spine fractures often happen when the rider gets pinned or crushed between vehicles and objects. This can cause temporary or permanent paralysis. Traumatic Brain Injury This is one of the most serious injuries sustained in a motorcycle crash. Traumatic brain injury - TBI is when the brain sustains trauma. These injuries usually happen when a motorcyclist is involved in an accident and is not wearing a helmet, their head hits an object forcefully, the head is shaken violently back and forth, or if the skull gets punctured. Around 15% of motorcyclists involved in accidents that receive medical treatment are diagnosed with a traumatic brain injury. When a person sustains a TBI, they can develop physical and cognitive deficits. Depending on the severity, brain injuries can be treated with surgery, traction, and rehabilitation, but can have lifelong effects. Organ Injury and Damage Intense and forceful impacts can cause internal organ damage. Internal bleeding is common in motorcycle accidents. This can be fatal if not diagnosed and treated. Injuries that prove to be fatal, more than three-quarters are caused by traumatic brain injury. Therapy Rehabilitation Our experienced team of accident physical therapists and chiropractic team will review the details of the collision, medical treatments and develop a thorough rehabilitation plan. Call our team today and let us help you put your life back together. Breakfast and Mental Health Beyond an individual's physical health, breakfast can significantly impact mood and mental health. According to a 2018 study, a healthy high-quality breakfast has been shown to reduce stress and depression in adolescents. Breakfast nutritional quality was based on individual responses to the following questions: - Do you have cereal or other grain-based products bread, toast, etc?
- Do you have some type of dairy product for breakfast?
- Do you have commercially baked goods like biscuits or pastries for breakfast?
If a participant stated they consumed commercially baked goods and did not eat bread/toast/cereal or dairy products for breakfast, this was considered a poor quality breakfast. Avoiding commercially baked goods altogether and eating whole bread, healthy cereals, and/or dairy products was considered a good quality breakfast. Choosing grain-based foods along with dairy products was considered healthy because these foods provide a wide range of nutrients. Healthy cereals can provide: - Protein
- Carbohydrates
- Micronutrients
Results found that individuals that ate healthy quality breakfasts had: - Reduced mental distress
- Reduced depressive symptoms
- Increased positive mood
- Improved quality of life
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Alicioğlu, Banu et al. “Motosiklet kazalarina bağli yaralanmalar” [Injuries associated with motorcycle accidents]. Acta orthopaedica et traumatologica turcica vol. 42,2 (2008): 106-11. Araujo, Miguel et al. “Effectiveness of interventions to prevent motorcycle injuries: a systematic review of the literature.” International journal of injury control and safety promotion vol. 24,3 (2017): 406-422. doi:10.1080/17457300.2016.1224901 Dupaix, John P et al. “A Comparison of Skeletal Injuries Arising from Moped and Motorcycle Collisions.” Hawai'i journal of health & social welfare vol. 78,10 (2019): 311-315. Elsemesmani, Hussein et al. “Association Between Trauma Center Level and Outcomes of Adult Patients with Motorcycle Crash-Related Injuries in the United States.” The Journal of emergency medicine vol. 59,4 (2020): 499-507. doi:10.1016/j.jemermed.2020.06.018 Peng, Yinan et al. “Universal Motorcycle Helmet Laws to Reduce Injuries: A Community Guide Systematic Review.” American journal of preventive medicine vol. 52,6 (2017): 820-832. doi:10.1016/j.amepre.2016.11.030
Baastrup’s syndrome is named after Christian Ingerslev Baastrup. He discovered and described the condition in 1933. In this syndrome, pain and inflammation are triggered when the spinous processes of two adjacent vertebrae begin to touch each other. This is where the term kissing spine came from. Most back and neck pain is attributed to inflammation or degeneration of the spinal vertebrae, discs, muscles, and nerves. This is a spinal condition that can cause problems with age. If experiencing pain that worsens when arching the back, consult a professional chiropractor. A physical examination and imaging could reveal the spine is going through this underdiagnosed condition. Kissing Spine Spine problems mostly involve the vertebrae and the discs. However, the spine has other components, which include spinous processes. These are thin segments of bone that protrude off the back of each vertebra. Kissing spine syndrome, also known as Baastrup’s disease, or interspinous bursitis, happens when these spinous processes begin to move close together and touch/kiss. Pain and inflammation can be triggered by this. It is believed to develop as a result of degeneration in the spine that comes with age. As vertebral discs break down from all the wear and tear of life, this can cause the spinous processes to move closer together and touch. This typically develops in the lumbar spine/lower back, but can also affect the cervical spine/neck. The most common symptom of kissing spine syndrome is back pain that worsens when touched or arching the back. For some individuals slumping forward or rounding the back, can help diminish the pain. When the spinous processes touch, they begin abrasively rubbing against each other. This wears them down and can lead to other types of spinal degeneration. Over time secondary problems can begin to present including neurological conditions caused by compressed nerves. The condition is common in older adults from the natural wear and tear on their spines. But young individuals specifically athletes, can develop the syndrome. - Poor posture
- Obesity
- Spinal injury/s are additional risk factors.
Diagnosing the condition involves a physical exam and imaging scans to confirm that the spinous processes are in fact touching. Chiropractic Care A chiropractor can help manage the pain caused by degenerative disc disease and kissing spine syndrome. Treatment protocols for kissing spine syndrome include: - Spinal adjustments
- Physical therapy massage
- Spinal manipulation
- Stretches
- Exercises
- Anti-inflammatory diet
Spinal decompression techniques can open the spinal segments so that the spinous processes don't touch. Manipulations can facilitate proper joint mobility and alleviate inflammation. Physical therapy exercises and stretches will help stretch the spine and the supportive tissues. If experiencing neck or low back pain, contact Injury Medical Chiropractic and Functional Medicine Clinic. Our spine specialists will listen, discuss, and develop a personalized treatment plan. We provide non-invasive approaches for long-term pain management and spinal correction for lasting comfort. The Paleo Diet The Paleo diet consists of eating foods that would have been available to humans before modern agriculture was established. If the food was not available to these human ancestors and they did not eat it, then it is not part of the Paleo diet. This includes eating: - Lean meats
- Fish
- Vegetables
- Fruits
- Eggs
- Nuts
The Paleo cuts out foods like: - Grains
- Legumes
- Dairy
- Sugars
- Processed oils
One study published in the American Journal of Clinical Nutrition compared the Paleo diet to other control diets based on United States nutritional guidelines. The researchers found that the Paleo diet generated improvements in waist circumference, triglyceride levels, and blood pressure. Disclaimer The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the musculoskeletal system’s injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, CTG*
email: coach@elpasofunctionalmedicine.com
phone: 915-850-0900
Licensed in Texas & New Mexico References Philipp LR, Baum GR, Grossberg JA, Ahmad FU. Baastrup’s Disease: An Often Missed Etiology for Back Pain. Cureus 8(1): e465. Published January 22, 2016. https://www.cureus.com/articles/3982-baastrups-disease-an-often-missed-etiology-for-back-pain. Accessed December 20, 2018. Filippiadis DK, Mazioti A, Argentos S, et al. Baastrup’s disease (kissing spines syndrome): a pictorial review. Insights Imaging. 2015 Feb; 6(1): 123–128. Published online January 13, 2015. https://link.springer.com/article/10.1007/s13244-014-0376-7 Accessed December 20, 2018.
Finding the right surgeon specializing in an individual's specific spinal conditions and physical health means doing some research. There are several types of procedures for spinal problems. The type of surgery depends on the condition and an individual's medical history. If surgery is recommended for a lumbar herniated disc or LHD combined with sciatica here are a few things to think about. Researching a spine surgeon First and foremost look for surgeons with: - Medical credentials like are they board-certified or board-eligible
- Completed a fellowship in spine surgery
- Devotes at least 50% of their practice to spinal conditions
- Specializes in treating herniated disc/s and sciatica. This means they will have added/specialized knowledge and expertise.
It is extremely important that an individual feels comfortable and feels they are able to communicate freely with the surgeon. A professionally qualified surgeon should: - Spend adequate time with the individual
- Answer all questions
- Provide all information needed about the condition and treatment
- Listen to what the individual has to say
- Is open-minded
- Is not hard to get in contact with
- Has experience in the latest methods and techniques
What to look at and think about Individuals can feel uncomfortable asking questions, but thorough communication is key. Remember, it is your body, and it is your right to know the details of the spinal disorder, along with non-surgical and surgical approaches to treatment that are available. There is time to consider the options and make an informed decision about the treatment plan as most spinal procedures are elective. Ask the surgeon all the questions you have to help decide wisely and with confidence. Make sure they address all concerns, and any others not listed. The surgeon's specialization/focus Orthopedic surgeons and neurosurgeons perform spinal procedures. Each will have a specific interest and expertise in certain spinal condition/s. For example, some surgeons may specialize in treating adult or pediatric patients, and some may only treat either lumbar/low back or cervical/neck conditions. Within those groups, some focus on: - Spinal deformities
- Tumors
- Myelopathy a spinal cord disease
- Specific spinal cord diseases
Minimal invasive surgery option Minimally invasive spine involves tiny incisions, that reduces the recovery time needed to heal. With this type, individuals can be up and walking within hours after surgery. Unfortunately, not all conditions can take this approach. Is the surgery absolutely necessary, or can it be treated non-surgically? Sciatica and herniated discs can be quite painful and cause disability. Never rush into surgery just to relieve symptoms. As surgery can cause other types of pain symptoms and issues. Herniation and sciatica can be resolved with: - Chiropractic
- Physical therapy
- Medications
- Injections
- Lifestyle changes
- Diet adjustments
- Regular exercise
- Weight loss
However, if there are neurologic symptoms, like weakness in the leg, foot, numbness, or loss of bladder or bowel control - this is considered a medical emergency - then surgery is absolutely needed. The number of similar procedures performed The surgeon’s experience is very important. The more experienced, the better. Ask if they can refer to other patients who have had similar procedures. Recovery time Every patient is unique, as is the type of surgery, and recovery times. They all vary accordingly. General health, physical condition, and the severity of the disorder play a role in how long and how involved recovery time will be. Experienced surgeons can provide more specific answers concerning recovery/healing time. Complication rate All surgeries carry some risk of complication. Complication rates that are more than 10% is a red flag. Possible post-surgery complications. Infection rate Surgeons should have an infection rate lower than 10%. However higher rates do not always mean that surgeon is at fault as higher rates can come from performing highly complex procedures. Another reason for high infection rates could be the patients themselves like smokers or individuals with diabetes have increased risks for infection. However, do not feel uncomfortable asking the surgeon to explain a high infection rate. Decide to not opt for spine surgery As a surgeon produces a diagnosis, they should present a recommended treatment plan, including alternative treatments/therapies. Ask for another explanation of any part of the evaluation, diagnosis, or available treatment options. Get a second opinion A second opinion should be encouraged. A second opinion can reinforce the surgeon’s recommendations and offers a new perspective. The surgeon should be comfortable with a second opinion. This does not mean that the individual does not trust the surgeon. It does mean that there is considerable interest in achieving optimal health and making sure that surgery is the absolute right thing to do. Pass on surgeons that discourage or disapprove of second opinions and continue looking. Dr. Alex Jimenez’s Blog Post Disclaimer The scope of our information is limited to chiropractic, musculoskeletal, physical medicines, wellness, and sensitive health issues and/or functional medicine articles, topics, and discussions. We use functional health & wellness protocols to treat and support care for injuries or disorders of the musculoskeletal system. Our posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate and support directly or indirectly our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. We understand that we cover matters that require an additional explanation as to how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. The provider(s) Licensed in Texas& New Mexico*
Getting workers’ compensation for a back/spinal injury can be a daunting and overwhelming task. There are plenty of questions, and we have answers from both medical and legal professionals. Anyone can be affected by back pain at work. - Truck drivers
- Manual laborers
- Construction workers
- Hairstylists
- Automotive technicians
- Teachers
- Healthcare workers
- Foodservice workers
- Hospitality workers
- Office workers
Work-related back injuries can be prevented by paying attention to posture, taking standing/moving breaks, stretching out, and lifting properly. However, if back pain at work stems from a work injury individuals could be entitled to workers’ compensation benefits. Workers’ Compensation Workers' compensation is an insurance program that helps with and provides benefits and medical care for workers that have been injured or fallen ill resulting directly from their job. This means if an individual is injured at work, employers have negotiated to free themselves of a majority of the liability by paying for the treatment and recovery. Companies that employ five-hundred or more are able to manage their own workers’ compensation program. However, most workers’ compensation programs are managed by state governments. Every state has its own workers’ compensation program that employers pay into. The federal government handles the federal workers’ compensation program for federal employees. The program is funded by the employer with the cost not affecting an individual's paycheck. Workers’ Compensation Coverage Compensation programs are different throughout the country. Typically workers’ compensation pays for: - Initial emergency department
- Urgent care visit
- Diagnostic testing recommended by the emergency department
- Follow-up physician
- Surgical intervention
- Rehabilitation
Under workers’ comp back injury treatment/s are completely covered, meaning an individual does not have to meet a deductible or pay premiums, copayments, or coinsurance. Individuals continue to receive regular health insurance benefits from the employer. This could require a deductible, premiums, copays, and coinsurance. This is for the treatment of other health issues while receiving workers’ compensation care. If an individual is unable to work because of a workers' comp back injury, a worker can expect to be paid a base salary after taxes while being treated. Those whose salary is dependent on overtime creates a disadvantage. Workers’ compensation can mean a pay cut for these individuals. Workers’ comp pay depends on the state. Usually, there is a wage rate set by the state. High Risk for Back Injury on the Job Employees that are involved in physical labor like construction, factory work, and healthcare work have a higher risk of getting a back injury on the job. These injuries are often the result of: - Improper lifting techniques
- Repetitively turning
- Twisting while lifting
- Holding something heavy
- Lifting heavy objects above the head
- Using the back muscles instead of the hips and legs when lifting bending of the knees and bringing heavy objects close to the core
Truck drivers also have a higher risk of back injuries. Sitting for long periods and reduced physical activity contributes to the back muscles losing their strength, endurance, and cardiovascular ability. Then when unloading the cargo the stress on the spine is doubled. Injury Report A back injury should be reported to the supervisor or the company’s human resources department. Depending on the state, there is a statute of limitations to file an injury claim. For example, an individual has one year from the date of injury to file a workers’ compensation claim with the supervisor or human resources department. However, it is best to report the injury and seek medical attention as soon as possible after being injured at work. The longer the wait, the more the employer could dispute the legal validity of a workers’ compensation claim. Injury Qualification If injured at work, assume the injury will be covered by workers’ compensation. However, it is not always completely clear. An individual could be injured at a work-related cookout or working from home and trip down the stairs. These are gray areas and are very new as more people working from home. These kinds of workers’ comp claims are now starting to be seen. Whatever the event, report injury/s to the employer. If the situation is untraditional, there could be some back and forth with the employer. Spine Specialist Referal To receive work comp treatment patients with back injuries will be referred to an occupational therapy clinic. An occupational therapist or clinic will set up the treatment. This could include: - Chiropractic
- Medication
- Physical therapy
- Hydrotherapy
- MRI
- CT scan
- X-rays
For many that could be enough to get them back to work. If the initial treatments fail an individual could be referred to a spine specialist to set up an optimal treatment plan. A spine specialist could recommend additional therapy, medication, diagnostic imaging, spinal injections, or surgery. Occupational therapy usually goes on for four to six weeks before the individual is referred to a spine specialist. This all depends on the situation. Individuals can be referred immediately for specific spinal treatment or be told to wait for a specific time. It all depends on the medical situation. Employer and the Spine Specialist In most states, employers will request a copy of the treatment plan and spine surgeon’s clinical notes written about the case during office or telemedicine appointments. Doctors have to provide clinic notes and treatment plans to the human resources departments along with the workers’ compensation insurance carrier. Consistent, active communication goes on between the primary doctor, the company’s human resources department, and the insurance carrier. Note that workers’ compensation is exempt from HIPAA privacy regulations. Employers and the workers’ compensation insurance carrier have access to medical records related to the back injury. But medical information unrelated to the injury is restricted. Obtaining Workers’ Compensation From a Doctor Generally, no. Obtaining Workers’ comp is between the individual and their employer, not the doctor. Sometimes doctors are asked to determine if an individual's injury/s are work-related. This involves going through medical records but these requests are rare. Benefits Duration It depends on the case and where an individual lives. Every state is its own system. In some states, treatment can be ongoing for as long as treatment is needed and is consistent. What is highly recommended is meeting with a workers’ compensation attorney in your state when beginning the process to learn your rights and the process. This can help in preventing issues from popping up like an employer pressuring a worker to come back before a doctor has cleared them to return. Making Most of Workers’ Comp Keep appointments and be compliant with the doctor's treatment plan and recommendations. Be transparent with the doctor. Not telling them exactly what is happening will not help in their recovery. If there is an improvement from the treatment/s fantastic, but if there are minimal to no improvements be as descriptive as possible about what is happening and what does work. The goal is to work with a clinical team that can get an individual better back to work and normal activities. Dr. Alex Jimenez’s Blog Post Disclaimer The scope of our information is limited to chiropractic, musculoskeletal, physical medicines, wellness, and sensitive health issues and/or functional medicine articles, topics, and discussions. We use functional health & wellness protocols to treat and support care for injuries or disorders of the musculoskeletal system. Our posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate and support directly or indirectly our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. We understand that we cover matters that require an additional explanation as to how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. The provider(s) Licensed in Texas& New Mexico*
In today's workforce, many jobs place workers at a higher risk for a back injury. The list is pretty extensive and may surprise you! Individuals that have suffered a neck or back injury at work know the cost goes beyond lost wages. The impact of these injuries on employees, employers, and the economy is staggering.
In a report published by the Bureau of Labor Statistics, there were 2.8 million cases of non-fatal occupational injuries and in 2018. Of these cases, more than 50% lost time from work, transferred to a different job, or restricted work activity. Not all of these cases were spine-related injuries. However, 880,000 cases were back pain-related injuries.
The World Health Organization's International Labour Office says that the problem is global.
Musculoskeletal diseases are a very common part of 270 million non-fatal work/job accidents where employees missed at least 3 workdays. Risky Jobs Occupational safety experts gather all kinds of information that they factor. This includes job requirements, work environment, and work station set up. In compiling the list of risky occupations, here are some of the criteria: - Heavy physical work
- Forceful lifting movements
- Bending
- Twisting
- Awkward work postures
- Whole-body vibration
- Static work postures like standing/sitting but never changing position compounds the risks to workers.
Two occupations that lead the list of jobs placing workers at the highest risk are construction and nurses/nursing home workers. Workers in both of these jobs tend to share the under-reporting of work-related injuries. This happens as the employees fear they will lose their job and cannot afford to take any time off. Construction Workers Employees at a construction site are repeatedly lifting, bending, carrying, pulling, and tugging. These repetitive movements lead to overuse injuries and back strain/sprains are a common part of this. More than 30% of workers have to miss job time. Those that must climb ladders or work on scaffolds have a greater risk of falling. This is where some serious spinal injuries can occur, causing disability and sometimes being fatal. Nurses/Nursing Workers Nursing homes and employment opportunities are growing from elderly population growth. These workers are at high risk for back pain and spine injury. This comes from transferring patients' from their beds, bathtub, and bathroom facilities. All these actions require lifting, carrying, holding, pulling, pushing, and turning. The Bureau of Labor Statistics reports nearly all back and shoulder injuries are the result of moving patients. Warehouse Workers This is another job that requires lifting, along with using forceful movements, bending, twisting, carrying, and placing the body in awkward positions. Sometimes these workers have to drive a truck or an industrial vehicle that creates whole-body vibration. Continual exposure to vibration can cause backache and soreness that can lead to lost work time. Dentists and Surgeons Both of these professions involve prolonged standing, stooping, bending, and awkward body positioning. Not to mention the mental strain that diverts the doctor's attention to proper posture and body mechanics that results in injury and pain. Landscapers The American Chiropractic Association puts landscapers in the top 10 list of jobs that cause back pain. This job puts these workers at a greater risk for cumulative trauma disorders. All the tasks that a landscaper has to do that include hedge trimming, tree pruning, and planting. These actions/movements involve lifting, reaching, bending, and stooping. This is a perfect set up for an overuse back injury. Hand tools that get used over and over can cause painful conditions like carpal tunnel syndrome and thoracic outlet syndrome. Thoracic outlet syndrome is when the nerves and blood vessels become compressed between the neck and shoulder. Store Cashier Grocery and retail store cashiers require workers to stand in one place for a long time. This along with the repetitive motions of scanning, typing, opening, closing combined with bagging and lifting bags over and over can cause neck, shoulder, back, leg and foot pain. Over half of checkout workers complain of back pain. Other High-Risk Jobs - Airline crews meaning pilots, baggage handlers,
- Factory workers
- Bakers
- Bus
- Cab drivers
- Cable and telephone line installers
- Carpenters
- Electricians
- Hairstylists
- Plumbers
- Carpet installers/cleaners
- Dry cleaners
- Medical technicians
- Farmers
- Firefighters
- Police
- Maintenance workers
- Automotive technicians
- Office personnel
- Professional athletes
Job Injury Prevention We may not be able to instantly change our occupation, but there are steps to help prevent neck and back injuries. The key is workplace ergonomics and safety. Be proactive to help reduce workplace risk for neck and back injury and share what you learn with co-workers. NCBI Resources Injuries that are caused by repetitive movements often develop gradually. This is the time when the symptoms are mild and come and go, so the individual just works through it and doesn’t think about it. It’s not until the symptoms get very painful and debilitating that the individual realizes that something is wrong, and then they seek medical attention. Don’t wait, as soon as you feel a tingle, slight pinch, or a little soreness and you feel that it stems from your work’s repetitive movements, get in touch with a doctor or chiropractor before it becomes excruciating.
Low back pain is one of the most common ailments for people visiting a doctor or an urgent care clinic. When the back pain becomes intense it can get you thinking something is seriously wrong with your back. The doctor might offer an x-ray or MRI scan to put your concerns at ease. Fortunately, most cases for low back pain even acute pain improve within days or a few weeks. Most cases are remedied with chiropractic, physical therapy, heat/ice therapy and rest. And a lot of these cases do not require any form of spinal imaging. However, there are those reasons when X-ray, MRI, CT scans are necessary to figure out what's going on. - Strained muscle
- Sprained ligament
- Poor posture
These are typical causes of low back pain that can be painful and limit activities. Back Pain Lasting Longer Than 2/3 Weeks Subacute pain lasts between 4 and 12 weeks while chronic back pain lasts 3 months or longer. These are not indications of a serious low spinal condition. Less than 1% of people with low back pain are diagnosed with a condition that may require spine surgery like: X-rays or MRI's for Diagnosing Low Back Pain Doctors may recommend an x-ray or MRI if the low back pain was from a traumatic injury, like a: - Slip
- Fall
- Automobile accident
Other potential causes of low back pain may warrant medical imaging immediately or later on. The diagnostic process starts with the evaluation of the low back symptoms and how they relate to what was found during the: - Physical exam
- Neurological exam
- Medical history
A doctor utilizes these results to figure out whether the need for spinal imaging is necessary, along with the type of imaging test, x-ray or MRI and the timing to confirm a diagnosis. A Low Back X-Ray/MRI X-ray spinal imaging is best at detecting bony structural problems but not so great with soft tissue injuries. There are X-ray series that may be performed to diagnose vertebral compression fractures like. - Anterior
- Posterior
- Lateral views
MRI is a radiation-free test. MRI's create 3-D anatomical views of the spinal bones and soft tissues. A contrast dye like gadolinium is used to enhance and improve the quality of the images. The contrast is injected through an intravenous line in your hand or arm before or during the test. An MRI can evaluate neurological symptoms, like radiating pain or pain that develops after being diagnosed with cancer. Symptoms, Co-existing Medical Diagnoses, and Conditions that may Require Spine Imaging Neurological symptoms - Low back pain that radiates, fans out or downward into the buttocks, legs, and feet
- Abnormal reflexes in the lower body can indicate nerve disruption
- Numbness, tingling, and possibly weakness develop
- Inability to lift your foot aka foot drop
Co-existing medical diagnoses and conditions - Cancer
- Diabetes
- Fever
- Osteoporosis
- Previous spinal fracture
- Spine surgery
- Recent infection
- Immunosuppressant medication use
- Corticosteroid medication
- Weight loss
X-ray Radiation Exposure When undergoing an x-ray, the radiation not absorbed by the body creates the image. The radiation dose is the same amount every time you undergo an x-ray. Radiation to your entire body is measured through the millisievert (mSv) also known as the effective dose. The effective dose helps a doctor measure the risk for possible side effects of radiographic imaging: - CT scans use radiation as well
- Certain body tissues and organs in the lower back are sensitive to radiation exposure like the reproductive organs.
MRI Radiation-Free Why Not Just Use This Test All The Time MRI's cannot be used on all patients because of its powerful magnet technology. Pregnant women or individuals that have metal inside their body like a spinal cord stimulator, heart pacemaker, etc cannot be scanned with an MRI. MRI testing is also expensive, doctors do not want to prescribe unnecessary tests that increase costs. Or because of the fine detail that MRI's provide, sometimes a spinal issue can look serious but is not. Example: An MRI of the lower back reveals a herniated disc in a patient that has no back/leg pain or other symptoms. This is why doctors bring all of their findings like the symptoms, physical exam, and medical history to confirm a diagnosis and then create the custom treatment plan. Imaging Test Takeaways If low back pain begins to take its toll, listen to what the doctor recommends. They might not order a lumbar x-ray or MRI immediately but remember the aforementioned issues like neurological symptoms and co-existing medical conditions. But these tests do help in discovering the cause or causes of the pain. Remember this is to help get patients to their optimal health and pain-free.
Auto Accidents & Back Injuries The spine is a complex structure that consists of bone, muscle, tendons, ligaments, nerves and other tissues. Spine fitness is essential towards maintaining the body’s optimal performance as it functions to support an upright posture, provides flexibility to allow the body to bend and twist freely, and protect the spinal cord. While a healthy back can easily be taken for granted, a back injury or other type of complication may result in long-lasting consequences that could alter an individual’s aspect of daily life.
Unfortunately, back injuries are among the most common types of complications suffered after an automobile accident. Each day, thousands of individuals are involved in head-on, side-impact, and rear-end auto collisions, often leading to spinal injuries even during minor car crashes. Depending on the force of the impact, a single or multiple areas of the back may be affected. Automobile injuries can range from mild sprains and bruises to fractured vertebrae and spinal cord damage.
If you’ve had a car accident, it’s essential to take note of any symptoms of back pain, as there are a variety of spine complications which could result after experiencing an auto collision. Disc Herniation One type of spine injury among individuals who have suffered from an auto accident is a herniated disc, or a slipped/ruptured disc. Discs are small, sponge-like structures found within the spinal column which function as cushions to separate and protect the vertebrae from the others while providing the spine with smooth flexibility. The force from an auto accident impact can damage a disc, causing it to break or deform, affecting its ability to cushion the bones of the spine.
Furthermore, a damaged disc can also place unnecessary pressure directly on the nerves surrounding it, leading to symptoms of pain, numbness and weakness on the region of the body where the affected nerve travels to.
Disc injuries to the lower back frequently lead to a group of symptoms commonly referred to as sciatica, which is characterized by radiating pain, numbness and tingling sensations in the leg and/or buttock on either side, or occasionally, in both sides, depending on the type of injury. The symptoms associated with sciatica can be impairing and may worsen over time if left untreated. Auto Injury Back Pain
Spinal Cord Distress Spinal cord injuries occur from the impact of an automobile accident. It sends a direct blow to the spine, that damages the delicate bundle of nerves within it. The spinal cord is the most important structure between the body and the brain. It is a vital link between the brain and the body, functioning to carry essential information back-and-forth from the brain to the central nervous system, facilitating motor control and sensory function. Spinal cord injuries impair the brain’s ability to communicate effectively with the rest of the body, resulting in paralysis and/or lack of sensation in all or part of the body. The more severe an injury to the spinal cord is, the more of the body will be affected. Compression Fracture aka Bone Break Car accidents can also cause compression fractures. Compression fractures or cracks in the bones of the spine may cause the vertebrae to collapse and deform. This can permanently alter the shape and structure of the spine. Symptoms of a compression fracture include pain and postural changes as well as breathing difficulties. Due to the fact that compression fractures are common among older adults, many individuals mistake the symptoms for signs of aging or arthritis. An estimated two-thirds of compression fractures go undiagnosed. While cars are built to withstand the great force of a collision, the human body is not. The complex structures of the body, especially the spine, are vulnerable even in low speed collisions, resulting in injuries or conditions more often than not. An individual who’s been injured in an accident should seek immediate medical attention in order to diagnose any possible injuries or conditions as early as possible to begin treatment. Chiropractic care can effectively treat a variety of spinal complications, including auto injuries. Through the use of spinal adjustments and manual manipulations, a chiropractor can gradually help restore the individual’s natural mobility and flexibility, as well as progressively strengthen the structures surrounding the spine to relieve the symptoms and restore the individual’s lifestyle. Sourced through Scoop.it from: www.elpasochiropractorblog.com After being involved in an automobile accident, injuries inflicted to the spine can be a common complication for many individuals. From herniated discs to compression fractions, the force of an auto collision can place great amounts of stress on the complex structures of the spine, often leading to damage, injuries and even aggravate an existing condition.
For more information, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 . The Clinic & Crossfit: A Clients Story
Jacqulyn Quevas is up on her feet a lot as a hair stylist and she was searching for and overall become healthier and once she found Push-as-Rx ®™, her amazing journey began. The motivation and enthusiasm of the trainers at Push as Rx has greatly influenced Jacqulyn.
The clinic and PUSH-as-Rx ®™ system is leading the field with laser focus supporting our youth sport programs. The PUSH-as-Rx ®™ System is a sport specific athletic program of reactive agility, body mechanics and extreme motion dynamics. Through detailed and continued assessments of the athletes in motion and under stress loads offer a clear scientific picture of body dynamics. This system also has helped many athletes come back from injury faster, stronger, and ready to safely return to their sport without losing a beat after recovery. Results demonstrate clear improved agility, speed, decreased reaction time and advantageous postural-torque mechanics. PUSH-as-Rx ®™ offers specialized extreme performance enhancements to our athletes no matter the age. By Dr. Alex Jimenez Contact Us
Additional Articles
Chiropractic: A Safer Strategy than Opioids
After being involved in an automobile accident, whiplash is the most frequent type of injury commonly diagnosed by medical specialists. The common symptoms associated with whiplash are most often misdiagnosed and, as a result, the auto injury is generally not treated at the source but, recent studies have found a possible reason behind the chronic symptoms of whiplash. Over the past couple of years, various studies have found that whiplash injuries can cause hyper excitability of the central nervous system, otherwise known as the peripheral nerves. A team of researchers conducted a meta-analysis and systematic review of 27 different trials, analyzing the connection between whiplash and the central nervous system dysfunction. Hyper excitability refers to an excessive reaction to stimuli, in this case, the peripheral nerves are altered, often presenting a variety of symptoms leading to other peripheral nerve hyperexcitability disorder syndromes and further complications. The researchers concluded that there is compelling evidence pointing to central hyperexcitability in individuals who’ve suffered from chronic whiplash. In fact, these changes in the central nervous system could potentially make people with whiplash type injuries more sensitive to other types of pain. Through chiropractic adjustments and manual manipulation, a chiropractor can gradually treat your whiplash injury. Because spinal adjustments can soothe oversensitive nerves, chiropractic care can be a potentially effective treatment for whiplash to effectively ease pain and nerve hyperexcitability.
Thoracic outlet syndrome, or TOS, is a medical term used to describe a group of disorders which frequently occur when the nerves or blood vessels in the space between the collarbone and the first rib, known as the thoracic outlet, become compressed. Thoracic outlet syndrome symptoms can vary according to which structures are compressed. If there is an impingement of the nerves in the thoracic outlet, the signs and symptoms usually include numbness and tingling sensations in the arms, hands, and fingers, pain and soreness in the neck, shoulder, or hands, a weakened grip, and wasting in the fleshy base of the thumb, also known as Gilliatt-Sumner hand. If there is a impingement of the blood vessels in the thoracic outlet syndrome, the signs and symptoms usually include arm pain and swelling, discoloration of the entire hand, a single or multiple fingers, weak or no pulse in the affected arm, cold fingers, hands, or arms, upper extremity fatigue, and numbness or tingling sensations in the fingers. most commonly, thoracic outlet syndrome is often diagnosed as a result of an automobile accident. Individuals who are involved in auto collisions frequently experience injuries. Whiplash, defined as a neck injury resulting from an abrupt, back-and-forth jolt of the head, is a common injury resulting from auto accidents. Because whiplash type injuries involve damage or injury to the surrounding muscles, tendons, and ligaments of the neck, the irritation from the trauma to these structures often leads to compression of the nerves and blood vessels around the cervical region of the spine, resulting in thoracic outlet syndrome. If you suffered an auto accident and you’ve been experiencing symptoms of pain and discomfort, make sure to seek immediate medical attention to diagnose any possible complications and begin treatment as soon as possible. A chiropractor can often help determine the root cause of your symptoms and develop a treatment plan to help regain your health.
|



 Your new post is loading...
Your new post is loading...














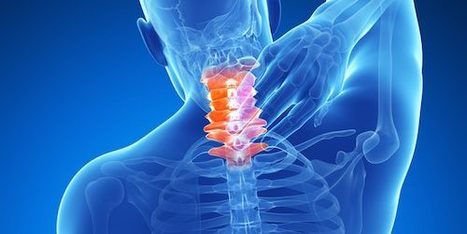



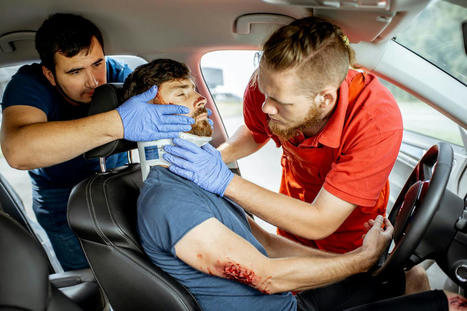













Wegovy ha cambiado vidas. Mido 6'3 ″ y comencé con 357 libras. He estado tomando este medicamento durante exactamente 4 meses y he perdido 60 libras.
https://acheterozempic5mg.com/
https://acheterozempic5mg.com/shop/
https://acheterozempic5mg.com/product/acheter-adipex-37-5-mg/
https://acheterozempic5mg.com/product/acheter-mounjaro-en-ligne/
https://acheterozempic5mg.com/product/acheter-ozempic-0-25/
https://acheterozempic5mg.com/product/acheter-ozempic-1mg/
https://acheterozempic5mg.com/product/acheter-ozempic-0-5-mg/
https://acheterozempic5mg.com/product/acheter-ozempic-2mg/
https://acheterozempic5mg.com/product/acheter-saxenda-en-ligne/
https://acheterozempic5mg.com/product/acheter-wegovy-en-ligne/
https://acheterozempic5mg.com/product-category/medicaments-contre-l...
https://acheterozempic5mg.com/product/acheter-de-loxycodone/
https://acheterozempic5mg.com/product/acheter-percocet-en-ligne/
https://ozempickopen.com/
https://ozempickopen.com/shop/
https://ozempickopen.com/product-categorie/weight-loss-medications/
https://ozempickopen.com/product/koop-ozempic-0-25mg/
https://ozempickopen.com/product/koop-ozempic-0-5mg/
https://ozempickopen.com/product/koop-ozempic-1mg-online/
https://ozempickopen.com/product/koop-ozempic-2mg-online/
https://ozempickopen.com/product/koop-adipex-online/
https://ozempickopen.com/product/mounjaro-kopen/
https://ozempickopen.com/product/saxenda-kopen/
https://ozempickopen.com/product/koop-wegovy-online/
https://ozempickopen.com/product/koop-zepbound-online/
https://ozempickopen.com/product/koop-rybelsus-online/
https://kaufenozemp25mg.com/
https://kaufenozemp25mg.com/geschaft/
https://kaufenozemp25mg.com/product/ozempic-kaufen-0-25mg/
https://kaufenozemp25mg.com/product/ozempic-kaufen-ohne-rezept-0-5-mg/
https://kaufenozemp25mg.com/product/ozempic-kaufen-schweiz-1mg/
https://kaufenozemp25mg.com/product/ozempic-kaufen-2mg-online/
https://ozempiccomprar1mg.com/
https://ozempiccomprar1mg.com/compra-ahora/
https://ozempiccomprar1mg.com/product/ozempic-comprar-sin-receta/
https://ozempiccomprar1mg.com/product/comprar-ozempic-online/
https://ozempiccomprar1mg.com/product/comprar-ozempic/
https://ozempiccomprar1mg.com/product/comprar-ozempic-2mg/
https://ozempiccomprar1mg.com/product/comprar-mounjaro-sin-receta/
https://ozempiccomprar1mg.com/product/comprar-saxenda-espana/
https://ozempiccomprar1mg.com/product/comprar-wegovy-en-linea/
https://ozempiccomprar1mg.com/product/comprar-metadona-en-linea/
https://acquistoozempic.com/
https://acquistoozempic.com/acquista-il-tuo-iniettabile-ozempic/
https://acquistoozempic.com/Prodotto/acquista-ozempic-0-25-mg/
https://acquistoozempic.com/Prodotto/acquisto-ozempic-senza-ricetta/
https://acquistoozempic.com/Prodotto/acquista-ozempic-1mg/
https://acquistoozempic.com/Prodotto/acquisto-ephedrine/
https://acquistoozempic.com/Prodotto/acquista-phentermine-online/
https://acquistoozempic.com/Prodotto/acquista-saxenda-online/
https://acquistoozempic.com/Prodotto/acquisto-wegovy-online/
https://acquistasubutexonline.com/
https://acquistasubutexonline.com/prodotto/
https://acquistasubutexonline.com/prodotto/acquista-ozempic-senza-p...
https://acquistasubutexonline.com/prodotto/acquista-saxenda-online/
https://acquistasubutexonline.com/prodotto/acquista-wegovy-in-italia/
https://acquistasubutexonline.com/prodotto/acquista-zepbound/
https://acquistasubutexonline.com/prodotto/acquista-subutex-online/
https://acquistasubutexonline.com/prodotto/acquista-methadone-in-it...
https://acquistasubutexonline.com/prodotto/acquista-actiskenan-online/
https://acquistasubutexonline.com/prodotto/acquista-morphine-online/
https://acquistasubutexonline.com/prodotto/acquista-ossicodone-online/
https://acquistasubutexonline.com/prodotto/efedrina-acquisto-online/
https://acquistasubutexonline.com/prodotto/acquista-vyvanse-online/
https://acquistasubutexonline.com/prodotto/acquista-methadone-in-it...
https://acquistasubutexonline.com/prodotto/acquista-adipex-online/
https://acquistasubutexonline.com/prodotto/acquista-victoza-online/
https://acquistasubutexonline.com/prodotto/acquista-qsymia-online/
https://buyozempiconlin.com/
https://buyozempiconlin.com/shop/
https://buyozempiconlin.com/product-category/weight-loss-medications/
https://buyozempiconlin.com/product/buy-ozempic-0-25mg/
https://buyozempiconlin.com/product/buy-ozempic-0-5mg/
https://buyozempiconlin.com/product/buy-ozempic-1mg-online/
https://buyozempiconlin.com/product/buy-ozempic-2mg-online/
Aeropuerto Adolfo Suárez Madrid-Barajas
@gmail.com
koop ozempic Nederland
koop ozempic voor gewichtsverlies
Koop pillen om af te vallen
koop ozempic 0.25 mg
acquista saxenda
acquista subutex online
acquista ozempic
acquista qsymia
koop ozempic Amsterdam
koop ozempic Rotterdam
koop ozempic Eindhoven
mounjaro koop
zepbound koop
rybelsus koop
saxenda koop
wegovy koop
acquisto ozempic
ozempic prezzo
acquistare ozempic 0.5mg
acquistare ozempic senza ricetta
acquistare ozempic 1mg
ozempic comprar 1mg
comprar ozempic 1mg
ozempic comprar sin receta
ozempic comprar online
ozempic comprar
comprar ozempic 2mg
comprar mounjaro
comprar wegovy
comprar saxenda
kaufen ozempic Deutschland
kaufen ozempic
kaufen ozempic 0.25 mg
kaufen ozempic 0.5 mg
kaufen ozempic 1 mg
kaufen ozempic 2 mg
acheter ozempic
Acheter Ozempic 0.25 mg
Acheter Ozempic 0.25 mg
Acheter Ozempic 0.5 mg
ozempic perte de poid
ozempic saxenda
ozempic wegovy en ligne
ozempic perte de poid
ozempic oxycodone en ligne
ozempic percocet en ligne
buy ozempic for WEIGHT
buy ozempic Florida
buy ozempic Canda
buy ozempic without prescriptions
buy ozempic 0.5 mg
buy ozempic 1mg
buy ozempic 2mg
acquista subutex online
acquista saxenda
acquista subutex
acquista victoza
acquista qsymia
acquista duromine
acquista methadone
acquista actiskenan
acquista morphine
acquista oxicodona
acquista sevredol
acquista dexedrine online
acquista pillole
acquista ritalin
acquista vyvanse
efedrina acquisto
acquista adipex
acquista belviq
acquista duromine
acquista ozempic
acquista qsymia