Your new post is loading...
 Your new post is loading...
It’s hard to tell from the data who’s still getting hospitalized with COVID. One frontline worker shares her observations.
Healthcare should not be limited by past decisions and most Australians would not be able to afford ‘astronomical’ cost of ICU, AMA says
ECMO uses an artificial heart and lung to replace the entire function of the person’s own heart and lungs outside the body. And COVID is demanding more ECMO than we’ve ever used before.
Healthcare workers on the sharp end of the pandemic are not just fighting a war against coronavirus, but combating a never-ending scourge of misinformation about the disease.
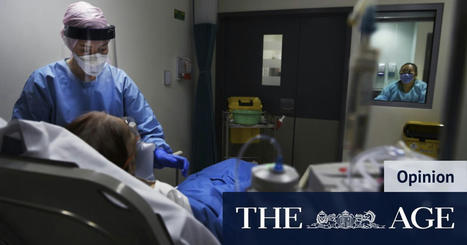
No one laughs. Bloody hell. These are really sick people. Everyone is on oxygen, there is coughing, spluttering, body aches. When I finally get into a room (gowned, gloved, goggles and visor on), I’m looking at a terrified person who has never seen me before and, I realise, doesn’t speak much English. Reassuring body language is hard. “I’m the doctor!” “You’re going to be all right!” Not that I actually know that. I do some gloved shoulder-squeezing to reassure, listen to the chest, feel the tummy and get out of there. You’re supposed to limit the time you are in the room.
A team from Stillwater Medical Center in Oklahoma tries valiantly to save the life of a man who needs an ICU bed. Will they find a bed for him before times runs out?
Kanak Patel, director of critical care medicine at Luminis Health Doctors Community Hospital in Lanham, Md., was relieved when the intensive care unit finally went down to zero patients with covid-19. But once the delta variant hit, he saw a return of patients, many unvaccinated, with severe illness because of the virus.
The mood at the Austin Hospital is one of trepidation. Staff are bracing for a volume of COVID-19 patients never before experienced in Australia.
The number of COVID patients needing an ICU bed in New South Wales is expected to keep climbing into October. The problem is that even now, with demand sitting well below the state's technical ICU capacity, hospitals are already feeling the strain. So what's the surge plan in New South Wales, and will it work the way the State Government is hoping? Featured: Dr Greg Fox, Professor of Respiratory Medicine at the University of Sydney, and respiratory physician, Royal Prince Alfred Hospital, Sydney
A short film offering a firsthand perspective of the brutality of the pandemic inside a Covid-19 I.C.U.
Last summer, when England's first peak of the coronavirus pandemic had subsided, Fazilah, an ICU nurse at a central London hospital, sat down to write her resignation letter.
While the number of people diagnosed with coronavirus continues to climb in Victoria, so too does the number of victims in intensive care, and the families behind the figures are struggling with the knowledge they may never be able to say goodbye.
Chief Health Officer says state can expect hundreds more seriously ill patients within the next fortnight.
|
I’ve seen people die without their family. It used to bring me to tears. Now I just feel weary
Most of the resources we are devoting to Covid in hospital are being spent on people who have not had jab, says an NHS consultant
Physical, mental and cognitive problems can last years after covid-19 or other severe illness is conquered
Who gets scarce life-saving resources when hospitals are overwhelmed? And how are these decisions made? State and territory governments are yet to answer these difficult questions.
We’ve cared for people in their 20s and 30s, and that has been confronting – most of my colleagues are the same age
A lot has changed in COVID treatment since the pandemic began. Here are the treatments you can expect — from being diagnosed, to going to hospital, and for those who need to be cared for in ICU.
The prediction came as Premier Daniel Andrews walked back a pledge to establish 4000 extra ICU beds in the state.
The term ‘intubation’ is used when experts talk about treating patients with severe COVID-19. But this medical term doesn’t explain the traumatic procedure involved.
Victorian intensive care specialists are gauging how many beds could be set up at short notice if the state's Delta outbreak explodes. It's a difficult balancing act involving staff fatigue and patients who will be forced to miss out on life-changing treatment.
Photojournalist Graeme Robertson has spent several days following two medical students and a consultant endocrinologist working on the Covid-19 ICU ward at the University College Hospital in London
In the event COVID-19 sees ICU resources stretched too thin, Victoria doesn't have clear, uniform or transparent guidelines outlining who should be prioritised for care.
As Victoria's COVID-19 cases surge, medical professionals in the state's Intensive Care Units are working tirelessly as the last line of defence to keep the critically ill alive.
|

 Your new post is loading...
Your new post is loading...
 Your new post is loading...
Your new post is loading...