 Your new post is loading...
 Your new post is loading...
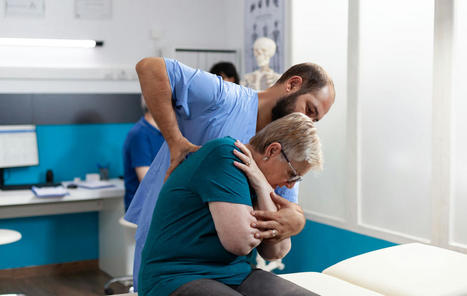
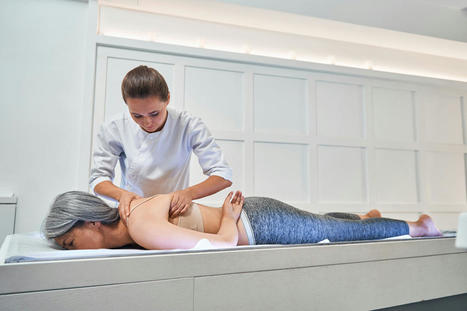
Nerve irritation occurs when the nerves exiting the spine become irritated and sensitized. Also known as nerve gliding restriction, it is a condition whereby a nerve becomes irritated by inflamed swelling of structures close to the nerve, such as joints, ligaments, muscles, or discs, that have sustained an accumulative strain which results in swelling and inflammation. A thorough chiropractic assessment and examination can diagnose the extent of the irritation and develop a personalized treatment plan. Nerve Irritation When swelling and inflammation interfere with the nerve root, the nerve transmits signals to the brain to let it know there is a threat. The brain interprets these signals and creates a protective response to avoid worsening the damage to the nerve. The protective reactions vary from person to person but can include the following: - Muscle tightness and guarding
- Aching sensation
- Cramping
- Radiating discomfort or pain
- Pins and needles
- Tingling
- Numbness
- Nerve root irritation also inhibits the body from recovering as fast as it should.
Nerve irritation is not to be confused with nerve root compression or radiculopathy. This is when the nerve becomes compressed/pinched, resulting in the loss of its functions like muscle strength and sensation. Sometimes individuals with nerve irritation can also experience increased neural tension. The nerves adapt to the mechanical loads placed on them through regular movements. Restrictions to neural mobility can cause symptoms to worsen along the pathway and distribution of the nerve. - The nervous system consists of the brain, spine, and nerve branches.
- The branches, similar to electrical cables, cannot stretch.
- Tension is generated when straightening out body areas, creating a pull and gliding of the nerve to the spinal cord.
- When nerve irritation occurs, signals are sent to protect the body, brain, spine, and branches.
Causes Most commonly, nerve irritation occurs when a structure adjacent to the nerve; this could be a joint, ligament, and/or muscle that accumulates strain and becomes dysfunctional, swollen, inflamed, and/or spasms resulting from protective guarding. - Mild nerve irritation can include accumulated strain from postural overload and swelling from a minor tear in an adjacent ligament.
- Often nothing shows as a problem on an MRI scan.
- Severe nerve irritation can include disc herniation and shows up on an MRI scan; surgery could be required in some cases.
Symptoms - Stiffness
- Tightness
- Aches
- Pains
- Persist even after days of rest, stretching, targeted exercises, avoiding movements, etc.
- Stretching feels good at first, but the pain returns or worsens a few hours later or the next day.
- The irritation blocks the effective recovery of muscle, joint, tendon, and ligament discomfort symptoms.
Chiropractic Care Treatment involves various therapies and strengthening the supporting structures while relaxing and releasing tight structures to avoid recurring injuries. Chiropractic care realigns the spine, corrects joints that have shifted out of place, helps to regulate the nervous system's function, and relieves irritation and inflammation. Whether in the form of an adjustment, traction, or guided exercise, all systems in the body are moved closer to a balanced state. This includes the: - Nervous system
- Immune system
- Respiratory system
- Circulatory system
- Endocrine system
- Skeletal system
- All help support the body's self-healing process and increase the nervous system's function.
The chiropractic team will guide the patient through the rehabilitation process to get back to full strength. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Ellis, Richard F, and Wayne A Hing. "Neural mobilization: a systematic review of randomized controlled trials with an analysis of therapeutic efficacy." The Journal of manual & manipulative therapy vol. 16,1 (2008): 8-22. doi:10.1179/106698108790818594 Gibson, William, et al. "Transcutaneous electrical nerve stimulation (TENS) for neuropathic pain in adults." The Cochrane database of systematic reviews vol. 9,9 CD011976. 14 Sep. 2017, doi:10.1002/14651858.CD011976.pub2 O'Shea, Simone D et al. "Peripheral muscle strength training in COPD: a systematic review." Chest vol. 126,3 (2004): 903-14. doi:10.1378/chest.126.3.903 Rozmaryn, L M et al. "Nerve and tendon gliding exercises and the conservative management of carpal tunnel syndrome." Journal of hand therapy: official Journal of the American Society of Hand Therapists vol. 11,3 (1998): 171-9. doi:10.1016/s0894-1130(98)80035-5 Sipko, Tomasz, et al. "Mobility of cervical spine and postural equilibrium in patients with spinal overload syndrome." Ortopedia, traumatologia, rehabilitacja vol. 9,2 (2007): 141-8.
Aging Arthritis: How the body changes as the years go by is determined by an individual's diet, physical activity/exercise, genetics, stress levels, sleep patterns, and self-care. As the body ages, natural degeneration from everyday wear and tear will present. The focus is on understanding how age-related degeneration can affect the body and what to do to prevent and treat it. Aging Arthritis Arthritis refers to joint inflammation and is the fundamental cause of various disorders that include: - Osteoarthritis
- Fibromyalgia
- Infectious arthritis
- Gout - metabolic arthritis
- Rheumatoid arthritis
- Lupus
- Childhood arthritis
Inflammation is just one symptom usually accompanied by swelling, pain, stiffness, immobility, and loss of function. Osteoarthritis - The most common type of arthritis is osteoarthritis, where the cartilage within joints begins to break down, and the bones begin to reshape.
- It's known as degenerative joint disease/wear and tear arthritis.
- The hands, hips, and knees are the most commonly affected joints.
- These changes often develop slowly but worsen if not treated.
- Symptoms include intense pain, stiffness, and swelling.
Fibromyalgia - Fibromyalgia is a condition that causes pain in various areas of the body, sleep problems, and fatigue.
- Individuals with fibromyalgia can be more sensitive to pain sensations.
- Treatments and management plans are available to help ease symptoms and restor function.
Infectious Arthritis - Infectious arthritis or septic arthritis is caused by an infection in the joints.
- Bacteria from another area of the body can invade a joint or the fluid surrounding it.
- Bacteria can enter the body from open wounds, injections, or surgery.
- Infectious arthritis is usually only present in one joint.
- Staphylococcus aureus is a bacteria that lives on healthy skin and is the cause of most infectious arthritis cases.
- A virus or fungus can also generate arthritic inflammatory symptoms.
Gout - Gout is a common type of arthritis that causes inflammation and pain.
- It usually only affects one joint, most commonly the big toe joint.
- Symptoms can intensify, known as flares, and other periods with no symptoms, known as remission.
- Recurrent gout episodes can degenerate into gouty arthritis, a more serious form of arthritis.
Rheumatoid Arthritis - Rheumatoid arthritis is an autoimmune and inflammatory disease in which the immune system attacks healthy cells, causing inflammation.
- Rheumatoid arthritis attacks numerous joints simultaneously, specifically in the hands, wrists, and knees.
- Rheumatoid arthritis causes the joint lining to become inflamed and starts to damage nearby tissues.
- Tissue damage that is severe or chronic enough can cause pain, balance problems, and visible deformities.
- Rheumatoid arthritis can also affect organs, like the lungs, heart, and eyes, by causing inflammation.
Lupus - Lupus is an autoimmune disease that affects various body systems.
- An autoimmune disease is when the immune system mistakes its tissues for bacterial, viral, or fungal intruders and attacks them.
- Lupus symptoms can be vague, making the disease hard to diagnose.
- The disease is known as the great imitator because symptoms can mimic other diseases.
- Symptoms range from mild to life-threatening.
- Seeing a rheumatologist is recommended, as they are specialists that can diagnose and treat arthritis, lupus, and other joint-related diseases.
Childhood Arthritis - Arthritis in children is known as juvenile or childhood arthritis.
- Juvenile idiopathic arthritis/juvenile rheumatoid arthritis is the most frequent form.
- The condition can cause long-term joint damage that can lead to disability.
Aging Arthritis and Chiropractic Care Chiropractic care is recommended for the treatment of any form of arthritis. Chiropractic care can work with other therapies to reduce swelling and inflammation, alleviate pain, and improve mobility and flexibility. - A chiropractor will utilize body imagery before beginning treatment.
- Imaging gives insight into the condition of the joints, and the visual, combined with a self-report from the individual, allows the chiropractor to create a personalized treatment plan.
- Once a chiropractor has identified which techniques the body can handle, treatment will commence that can include:
- Therapeutic massage
- Percussive massage
- Ultrasound
- Electrotherapy
- Low-level cold laser therapy
- Infrared heat
A chiropractor's objective is to rebalance, realign and strengthen the body, relieve pressure or stress at the junction of the joints, and expedite healing and rehabilitation. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Abyad, A, and J T Boyer. "Arthritis and aging." Current opinion in rheumatology vol. 4,2 (1992): 153-9. doi:10.1097/00002281-199204000-00004 Chalan, Paulina, et al. "Rheumatoid Arthritis, Immunosenescence and the Hallmarks of Aging." Current aging science vol. 8,2 (2015): 131-46. doi:10.2174/1874609808666150727110744 Goronzy, Jorg J et al. "Immune aging, and rheumatoid arthritis." Rheumatic diseases clinics of North America vol. 36,2 (2010): 297-310. doi:10.1016/j.rdc.2010.03.001 Greene, M A, and R F Loeser. "Aging-related inflammation in osteoarthritis." Osteoarthritis and cartilage vol. 23,11 (2015): 1966-71. doi:10.1016/j.joca.2015.01.008 Sacitharan, Pradeep Kumar. "Ageing and Osteoarthritis." Sub-cellular biochemistry vol. 91 (2019): 123-159. doi:10.1007/978-981-13-3681-2_6
Around the world, pain, especially chronic pain, is widespread to an individual. When the body goes through a tremendous amount of activity, the muscle tissues will rip and tear to strengthen the body for the next activity it overcomes. But when the muscle tissues tear and cause pain to the body, it can take a week or even months for the tissue to recover. Many recovery treatments can help alleviate the pain that a person is in, and one of the recovery treatments that most physicians use is low laser therapy. Low Laser Therapy & Musculoskeletal Pain Doctors have used low laser therapy to help patients alleviate pain and repair muscle tissue in the affected area of the body. Studies have found that the effects of low laser therapy had a positive impact on the treated area. The study showed that the low laser treatment has helped with relieving pain and has promoted tissue repair. The effects of the low laser wavelength have enhanced the healing process by promoting cell proliferation, causing pain relief. One of the efficient ways that low laser therapy is beneficial to the body is to alleviate musculoskeletal pain. Musculoskeletal pain is a variety of issues in the body. From muscle pain to fibromyalgia, it can render a person miss out on everyday activities, causing them to miss work or school. Studies have shown that when a patient is going in for low laser therapy, the effects from the laser wavelength can reduce inflammation and edema in the affected area. The studies even show that the laser light effects are photochemical and not thermal. The laser light will trigger a biochemical change in the body, causing the photons from the affected area to be absorbed, thus triggering a chemical change in the area. Efficient Uses of Low Laser Therapy Other studies even show that the low laser wavelength triggers chemical alterations and potential biochemical benefits to the human body. This means that if a person is suffering from chronic pain when going for low laser treatment, the laser can relieve chronic pain symptoms and even osteoarthritic conditions. Another efficient use of low laser therapy is that it can suppress the MMP or mitochondrial membrane potential in the DRG neutron while reducing adenosine triphosphate or ATP production in the body. In other words, the effects of low laser therapy can suppress and reduce inflammation receptors in the body, thus causing long-term results that last for years, improving tissue healing. Another efficient way low laser therapy is beneficial is that it can be combined with light exercises as a staple of rehabilitation. Studies have found that the combination of low laser therapy and exercise has merit. When an individual combines stretches and low laser therapy as part of their rehabilitation, the data shows a reduction in pain symptoms and fatigue in the body. Conclusion All in all, the efficient effects of low laser therapy are beneficial by reducing inflammation and damping the pain receptors in the body. Since chronic pain is worldwide and can cause harmful effects to the body, using low laser therapy can dampen the pain receptors. Having low laser therapy treatments as part of their daily regime and light exercises for anyone with chronic pain can get their body moving pain-free. Since the body goes through so much, having low laser therapy is one of the many recovery treatments that can provide long-lasting results and promote overall wellness. References: Cotler, Howard B., et al. “The Use of Low-Level Laser Therapy (LLLT) for Musculoskeletal Pain.” MOJ Orthopedics & Rheumatology, U.S. National Library of Medicine, 9 June 2015, www.ncbi.nlm.nih.gov/pmc/articles/PMC4743666/. Dima, Robert, et al. “Review of Literature on Low-Level Laser Therapy Benefits for Nonpharmacological Pain Control in Chronic Pain and Osteoarthritis.” Alternative Therapies in Health and Medicine, U.S. National Library of Medicine, 24 Sept. 2018, pubmed.ncbi.nlm.nih.gov/28987080/. Enwemeka, Chukuka S., et al. “The Efficacy of Low-Power Lasers in Tissue … – Medical Laser.” Medical Summus Laser, 2004, medical.summuslaser.com/data/files/77/1585165534_SpHfd8kFyVara63.pdf. Kingsley, J. Derek, et al. “Low-Level Laser Therapy as a Treatment for Chronic Pain.” Frontiers, Frontiers, 19 Aug. 2014, www.frontiersin.org/articles/10.3389/fphys.2014.00306/full. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico*
Although it is not officially summer, the past few weeks sure feels like it. Especially for those with joint discomfort and pain. As the body ages, individuals may notice their joints have some mobility/flexibility issues in the summer heat. Again, the heat and humidity are the culprits. The hotter it is, the more the body is susceptible to inflammation and swelling. The more prone an individual's body is to swelling, the more pain can present. Barometric pressure can also have some form of impact on joint health. The pressure changes can cause the joints to become more sensitive. When the pressure changes, individuals often speak of their joints feeling tighter combined with stiffness, leading to a cycle of swelling and pain. Joint Anatomy Whether it’s the hip, knee, elbow, or hand, all of the body's joints have fluid in them. It is a gel-like substance known as synovial fluid. This is what lubricates the joints and keeps them functioning smoothly. However, the temperature and humidity levels can change the thickness of the fluid in the joints. This means that the synovial fluid can become inflamed with the weather changes. This is a symptom when the joints begin to feel like they cannot move and/or are becoming stiff. Joint inflammation can become more common and chronic as the body gets older. Weather and the joints The summer heat and humidity can affect the joint because: - The tendons, ligaments, and muscles expand in this type of weather
- The heat can restrict individuals from moving around. Non-use stiffens the joints
- Joints that have worn down cartilage could have exposed nerves that are reacting to the temperature changes
- Humidity causes the body to lose water by sweating. This can reduce the fluid around the joints leading to stiffness, immobility, and pain.
However, not everyone has joint problems in the summer heat. Many have joint issues when it's cold, damp, or raining. Other's are at their best in cool, dry weather. It depends on an individual's body and how their joints react when the temperature changes. Maintaining joint health for the summer heat When joint discomfort or pain presents in the summer, there are a few easy ways to gain relief. Properly Hydrate the Body Water and sports drinks maintain the fluid levels in the body, specifically, it keeps the joints moving. One way to hydrate the body can be achieved by eating healthy fruits and vegetables. Water-rich fruits and vegetables include: - Watermelon
- Oranges
- Strawberries
- Tomatoes
- Cucumbers
- Spinach
- Celery
Over-The-Counter pain ointments and creams Arthritis and anti-inflammatory creams/ointments can ease joint pain by allowing more blood circulation in the affected areas. Dressing for the heat Wear loose, natural fiber, breathable clothing that allows the body to move freely while maintaining a cool temperature. Relax in the air conditioning Get into the air conditioning. The cool air can help reduce joint inflammation. Get in the Water Swimming or just wading through doing some light exercise in the water cools the body’s core. In addition, the buoyancy of the water relieves pressure on the joints. Body Water The body is made up of as much as 2/3's water. Even though much of the body is made up of water, body composition changes based on functional needs. Essential functions of water include: - Water is the building block to almost every cell in the body
- It regulates the body's temperature through sweating and respiration
- Carbohydrates and proteins for energy are transported via the water in the blood
- Water assists in the removal of metabolic waste through urination
- It is part of the shock-absorbing system that protects the brain and spinal cord
- Water is part of the saliva and fluid that lubricates the joints
The amount of water in the body depends on various factors. This includes: - Age
- Gender
- Physical activity
- It is referred to as Total Body Water or TBW.
TBW is constantly changing with gains and losses of fluid in healthy adults. The body can detect irregularities and compensate for losses and/or gains to ensure that the systems are balanced. General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. In addition, we provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Morton, Darren, and Robin Callister. “Exercise-related transient abdominal pain (ETAP).” Sports medicine (Auckland, N.Z.) vol. 45,1 (2015): 23-35. doi:10.1007/s40279-014-0245-z Peeler, Jason et al. “Managing Knee Osteoarthritis: The Effects of Body Weight Supported Physical Activity on Joint Pain, Function, and Thigh Muscle Strength.” Clinical journal of sports medicine: official journal of the Canadian Academy of Sports Medicine vol. 25,6 (2015): 518-23. doi:10.1097/JSM.0000000000000173 Quick, D C. “Joint pain and weather. A critical review of the literature.” Minnesota medicine vol. 80,3 (1997): 25-9. Timmermans, Erik J et al. “The Influence of Weather Conditions on Joint Pain in Older People with Osteoarthritis: Results from the European Project on OSteoArthritis.” The Journal of rheumatology vol. 42,10 (2015): 1885-92. doi:10.3899/jrheum.141594
How often do you feel more susceptible to pain, discomfort, and inflammation? Rheumatoid arthritis (RA) is an autoimmune disease that affects about 0.5 to 1.0 percent of the adult population throughout the world. Evidence suggests that the autonomic nervous system (ANS) plays a fundamental role in the management of an abnormal immune response and inhibition of inflammation. The ANS regulates cytokine production through the cholinergic anti-inflammatory pathway, including the efferent vagus nerve, the neurotransmitter ACh, and its receptors (α7 nicotinic ACh receptor, α7 nAChR). Turmeric, or curcumin, has historically been utilized as a spice and a medicinal herb in India and China. Evidence suggests that curcumin affects diverse bioactivities. In recent years, a variety of research studies have shown that consuming curcumin considerably ameliorated collagen-induced arthritis (CIA). A clinical trial has shown that curcumin is a safe and effective natural remedy for RA patients. However, pharmacokinetic research studies have shown that its bioavailability can be very poor which raises the question, how does curcumin, or turmeric, produce an anti-inflammatory effect?
Of all of the wide array of health issues that healthcare professionals talk to their patients about, there is one which is tremendously overlooked and not taken seriously: brain fog. Many people suffer from brain fog and fatigue and unfortunately, many people are left to fend for themselves when it comes to this health issue. Patients describe feeling as if they’re living in a haze, their lives passing them by. Instead of being engaged in the present moment, patients describe feeling as though they’re seeing life from a distance. Their thinking is no longer sharp, and their brilliant minds are sidelined. Why do health issues like these fall through the cracks of conventional medicine? This may be because there’s currently no definitive treatment available for brain fog. The purpose of the following article is to discuss the causes of inflammation and brain fog. Understanding the reasons for this type of health issue may hopefully help shine a new light on future treatments. Brain Fog and Inflammation Inflammation is an essential part of the immune system. We need inflammation to protects us from injury, infection, and illness. However, as with everything else in the human body, it is all about balance. An excessive amount of inflammation can cause the blood-brain barrier (BBB) to become more permeable, leading to brain inflammation. Neuroinflammation is sometimes known as “leaky brain syndrome” and this inflammatory oxidative stress (OS) in the hypothalamus of the brain is ultimately believed to be the root cause of brain fog, among other neurological diseases, such as Alzheimer’s disease.
|
Neck injuries and whiplash symptoms can be minor and go away within a few days. However, whiplash symptoms can manifest days later and become varied and chronic, ranging from severe pain to cognitive problems. These are collectively called whiplash-associated disorders because of the varied complexity of the symptoms. A common condition is a whiplash nerve injury. These injuries can be severe and require chiropractic treatment. Whiplash Nerve Injury Surrounding muscles, tissues, bones, or tendons can cause a whiplash nerve injury. The neck's spinal nerve roots become compressed or inflamed, leading to cervical radiculopathy symptoms of tingling, weakness, and numbness that can radiate down the shoulder, arm, hand, and fingers. Typically, cervical radiculopathy is only felt on one side of the body, but in rare cases, it can be felt on both sides if more than one nerve root is affected. Neurological Cervical Radiculopathy - Neurological problems can become severe and can reduce the ability to perform many routine tasks, such as gripping or lifting objects, writing, typing, or getting dressed.
Cervical radiculopathy involves one or more of the following neurological deficiencies. - Sensory - Feelings of numbness or reduced sensation. There can also be tingling and electrical sensations.
- Motor - Weakness or reduced coordination in one or more muscles.
- Reflex - Changes in the body's automatic reflex responses. An example is a diminished ability or reduced hammer reflex exam.
Symptoms Because every case is different, symptoms vary depending on the location and severity. Symptoms can flare up with certain activities, like looking down at a phone. The symptoms then go away when the neck is upright. For others, symptoms can become chronic and do not resolve when the neck is resting and supported. Common symptoms include: Fatigue - Decreased energy levels could be related to sleep problems, depression, stress, pain, concussion, or nerve damage.
Memory and/or concentration problems - Cognitive symptoms could involve difficulty with memory or thinking.
- Symptoms can start shortly after the injury or not appear until hours or days later.
- Cognitive problems could be from a brain injury or related to various types of stress.
Headaches - This could be neck muscles tightening or a nerve or joint becoming compressed or irritated.
Dizziness - Dizziness could be from neck instability, a concussion/mild traumatic brain injury, and nerve damage.
Vision problems - Blurry vision or other visual deficits could result from any number of causes, including concussion or nerve damage.
- Vision problems could also contribute to dizziness.
Ringing in the ears - Also called tinnitus, this can be ringing or buzzing in one or both ears and can range from intermittent and minor to constant and severe.
- Whiplash complications such as injury to the brain region that controls hearing, nerve or vascular damage, jaw injury, or stress can lead to tinnitus.
Chiropractic Care The appropriate chiropractic treatment is unique to each whiplash nerve injury and is directed at the primary dysfunctions detected during the initial examination. A personalized treatment plan addresses factors in an individual's work, home, and recreational activities. Treatment includes: - Massage manual and percussive for nerve and muscle relaxation
- Decompression therapy
- Nerve release techniques
- Targeted stretches and exercises
- Ergonomics
- Health and nutritional recommendations
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified healthcare professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and directly or indirectly support our clinical scope of practice.* Our office has reasonably attempted to provide supportive citations and identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, don't hesitate to get in touch with Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Goldsmith R, Wright C, Bell S, Rushton A. Cold hyperalgesia as a prognostic factor in whiplash-associated disorders: A systematic review. Man Ther. 2012; 17: 402-10. McAnany SJ, Rhee JM, Baird EO, et al. Observed patterns of cervical radiculopathy: how often do they differ from a standard "Netter diagram" distribution? Spine J. 2018. pii: S1529-9430(18)31090-8. Murphy DR. History and physical examination. In: Murphy DR, ed. Conservative Management of Cervical Spine Syndromes. New York: McGraw-Hill, 2000:387-419. Shaw, Lynn, et al. “A systematic review of chiropractic management of adults with Whiplash-Associated Disorders: recommendations for advancing evidence-based practice and research.” Work (Reading, Mass.) vol. 35,3 (2010): 369-94. doi:10.3233/WOR-2010-0996 Travell JG, Simons DG. Myofascial Pain and Dysfunction: The Trigger Point Manual. Vol. 1, 2nd ed. Baltimore, MD: Williams and Wilkens, 1999.
Muscle spasms also referred to as muscle cramps, are painful contractions and tightening of the muscles. They are common, involuntary, and unpredictable. Temperature drops and cold weather can cause the muscles and joints to contract and tighten, leading to spasms and pain. Chiropractic, physical therapy massage, exercises, stretching, and an anti-inflammatory diet can bring relief and help strengthen the muscles to prevent future episodes. Muscle Spasms Spasms are common and can affect any of the muscles. They can involve part of a muscle, all of a muscle, or several muscles in a group. Spasms occur when the muscle/s involuntary and forcibly contract uncontrollably and are unable to relax. The most common sites for muscle spasms include: - Hands
- Arms
- Abdomen
- Back
- Legs
- Thighs
- Calves
- Thighs
- Feet
How Cold Affects the Muscles As the weather gets colder, this causes the muscles in the body to lose heat, causing them to contract. As a result, the muscles and joints become tighter, stiffer, and decrease mobility and range of motion. This forces the muscles to work harder than usual to compensate. This can increase the fatigue of the muscles, leading to more prolonged bouts of pain and discomfort after physical activity, movement, exercise, etc. Symptoms and Causes A cramp can last a few seconds or last up to 15 minutes. During a muscle spasm, the following may be experienced: - Twitching in the muscle.
- Pain in the muscle.
- Throbbing.
- Hardness and/or stiffness.
- The muscles appear physically distorted.
Because the muscles have to work harder, the cold weather can increase muscle spasms. One of the most common causes of muscle spasms is overuse and fatigue. However, exact causes vary from person to person. Some experts believe that one or more of the following contribute to the spasms/cramps, and they include: - Dehydration.
- Stress.
- Not stretching the body regularly.
- Muscle fatigue.
- Restricted blood circulation.
- Involuntary nerve discharge/s.
- Over-exercising.
- Exercising in the heat.
- Exhaustion of salts and minerals:
- Potassium
- Magnesium
- Calcium
Possible causes for leg cramps at night or nocturnal leg cramps specifically include: - Sitting for too long without moving around to keep circulation healthy.
- Sitting with unhealthy posture.
- Overusing the muscles.
- Standing or working on hard floors.
Dealing With The Cold One way to deal with the cold is to warm up before any physical activity. Taking a few minutes to get the heart rate up can increase the blood flow and flexibility of the muscles. This will ensure the muscles are functioning correctly and avoid the need to work harder to stop spasms. When a cramp strikes, there are a few steps to try to alleviate the spasm: - Stretching the affected area.
- Massaging the affected area manually with a massage roller, percussive massager.
- Stand up.
- Move around.
- Apply heat or ice.
- A warm bath, shower with massage setting if possible.
- Ibuprofen and acetaminophen.
- Vitamin B12 complex can help prevent cramps.
Getting Back To Fitness Get back into regular exercising with a few tips for making the transition as smooth as possible. Start Slow - Don't try to jump back into exercise in attempting to crush out a challenging workout.
- Commit to a few light workouts a week that integrate stretching pre and post-exercise.
- Over-exerting the body increases the risk of injuries, motivation loss, and prolonged exhaustion.
Create a Workout Schedule That Works For You - Routines and habits can help stay on track.
- Build a sustainable exercise routine to stay focused and committed.
- Find times that work.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References American Academy of Orthopaedic Surgeons. Muscle Cramp. (http://orthoinfo.aaos.org/topic.cfm?topic=A00200) Accessed 3/1/2021. American Association of Osteopathy. Muscle Cramp—A Common Pain. (http://www.osteopathic.org/osteopathic-health/about-your-health/health-conditions-library/general-health/Pages/muscle-cramp.aspx) Accessed 3/1/2021. Herzberg J. Stevermer J. Treatments for Nocturnal Leg Cramps. (https://www.aafp.org/afp/2017/1001/od3.pdf) Am Fam Physician 2017;96(7):468-469. Accessed 3/1/2021. Young G. Leg Cramps. (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4429847/) BMJ Clin Evid 2015; May 13;1113. Accessed 3/1/2021.
Polymyositis is a disease that causes the body's muscles to become irritated and inflamed. It can affect the muscles all over the body. The muscles gradually begin to break down and weaken, making everyday movements difficult. This disease falls into a category known as inflammatory myopathies. Polymyositis Unknown Causation The causes of polymyositis are currently unknown. However, experts believe it could be associated with or triggered by a virus or an autoimmune reaction. An autoimmune response is when the body attacks itself along with the body's tissues. It's seen in individuals ages 31 to 60 and is rarely seen in individuals younger than 18. In some instances, medication can lead to an allergic reaction/response that causes muscle irritation and damage. But in most cases, healthcare experts are not able to find the exact cause. Symptoms The condition can affect the muscles all over the body. Physical activities like walking, getting up from a chair, or lifting objects can become difficult to perform. It can also affect the muscles that allow for eating and breathing. The muscles at the center of the body tend to be affected the most. Common symptoms include: - Muscle pain.
- Muscle stiffness.
- Muscle weakness, specifically in the abdomen, shoulders, upper arms, and hips.
- Joint pain and stiffness.
- Breathing problems.
- Problems swallowing.
- Abnormal weight loss can become an issue if there are problems with swallowing.
- Irregular heart rhythms if the heart muscle/myocardium becomes inflamed.
- Individuals may notice they have trouble climbing stairs or lifting their arms.
- The inflammation can worsen, causing pain and weakness that affects the wrists, lower arms, and ankles.
Diagnosis Diagnosis begins with the individual's medical history, family medical history if necessary, and a physical examination. The examination includes seeing and feeling the strength of the muscles. Tests will be required that include: Blood Tests - Blood tests allow the doctor to see if there are signs of muscle inflammation.
- They also show if there are abnormal proteins that form in autoimmune diseases.
Electromyogram EMG - This test can be used to find abnormal electrical activity in the affected muscles.
MRI - Magnets and computer graphic imagery are used to help the doctor inspect for inflammation in the body.
Muscle Biopsy - A small piece of muscle tissue is removed to be analyzed with a microscope.
Treatment Treatment depends on how severe the condition is, individual symptoms, age, and overall health. Currently, there is no cure for polymyositis, but symptoms can be managed. Individuals are recommended to utilize more than one type of treatment because the treatment plan may also need to be changed as treatment progresses. Treatments include: Anti-inflammatory Medication Steroid medication can help manage the disease and reduce symptoms, and corticosteroids can help ease inflammation in the body. The symptoms improve within 4 to 6 weeks, and a healthcare provider can lower the dosage after the symptoms decrease to reduce and ease any side effects. Immunosuppressive Medication - These medications block or slow down the body's immune system responses.
- Talk with a doctor about the risks, benefits, and side effects of all medications.
Chiropractic and Physical therapy - Chiropractic treatment and physical therapy can help:
- Aligning the spine to provide optimal nerve energy and blood circulation.
- Therapeutic massage to stimulate and keep the muscles loose.
- Specific exercises to help stretch and strengthen the muscles.
- These can help keep the muscles from shrinking.
Heat therapy and Rest - Heat therapy and allowing the body to rest thoroughly can help decrease pain symptoms.
Special Braces - Body, hip, and leg braces can help support the muscles and help with mobility.
Complications Polymyositis left untreated can lead to severe complications. The muscles become weaker, increasing the risk of falling and limiting daily activities. - If the chest muscles are affected, there could be problems with breathing that can lead to respiratory failure.
- If the digestive tract is affected, malnutrition and unintentional weight loss can result.
- Polymyositis poorly managed well can cause severe disability.
Nutrition and Muscle Growth Protein - Protein is the foundation for gaining muscle.
- This essential component is for all of the body's daily functions.
- It is essential to balance protein increase with overall diet.
- Carbs are the body's fuel source.
- Carbs should be a daily element of nutritional intake because they are the primary component.
- Acquiring energy
- Preventing muscle weakness and degradation
Consuming Carbs - Understanding how accurate results only happen when both sides work together.
- Healthy consumption of protein and carbohydrates can help muscle growth and sustain optimal health for all body types.
General Disclaimer * The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the injuries or disorders of the musculoskeletal system. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. Dr. Alex Jimenez DC, MSACP, CCST, IFMCP*, CIFM*, ATN* email: coach@elpasofunctionalmedicine.com Licensed in: Texas & New Mexico* References Corrado, Bruno et al. “Supervised Physical Therapy and Polymyositis/Dermatomyositis-A Systematic Review of the Literature.” Neurology international vol. 12,3 77-88. 24 Nov. 2020, doi:10.3390/neurolint12030015 Findlay, Andrew R et al. “An overview of polymyositis and dermatomyositis.” Muscle & nerve vol. 51,5 (2015): 638-56. doi:10.1002/mus.24566 Sasaki, Hirokazu, and Hitoshi Kohsaka. “Current diagnosis and treatment of polymyositis and dermatomyositis.” Modern rheumatology vol. 28,6 (2018): 913-921. doi:10.1080/14397595.2018.1467257 Van Thillo, Anna et al. “Physical therapy in adult inflammatory myopathy patients: a systematic review.” Clinical rheumatology vol. 38,8 (2019): 2039-2051. doi:10.1007/s10067-019-04571-9
How often do you get irritable, shaky, or have light-headedness between meals? How often do you have difficulty concentrating before eating? How often do you feel agitated, easily upset, and nervous between meals? Many researchers and healthcare professionals believe that your brain and gut are connected. Moreover, recent research studies have demonstrated that the brain can affect gut health and the gut can affect brain health. The communication system between your brain and gut is known as the gut-brain axis. In the following article, we will discuss the gut-brain axis. Understanding the Gut-Brain Axis The gut-brain axis is the communication network that connects your gut and brain. These two fundamental organs are both physically and biochemically connected in a variety of different ways. The neurons and the vagus nerve are essential for the brain and central nervous system (CNS). There are approximately 100 billion neurons in the human brain. The gut itself also contains about 500 million neurons, all of which are connected to the brain through nerves found in the nervous system. The vagus nerve is one of the largest nerves connecting the gut and brain. It sends signals in both directions. By way of instance, in several animal research studies, stress can ultimately affect the signals sent through the vagus nerve and it can also cause gastrointestinal health issues. Another research study conducted on humans found that people with irritable bowel syndrome (IBS) or Crohn’s disease had decreased vagal tone which suggests the decreased function of the vagus nerve. One research study in mice found that feeding them a probiotic reduced the amount of stress hormone in their blood. According to the research study, however, when the vagus nerve was cut, the probiotic had no effect. The brain and gut are also ultimately connected through chemicals known as neurotransmitters. Neurotransmitters created in the brain help regulate mood, including feelings and emotions. Furthermore, the neurotransmitter known as serotonin can help manage happiness and it also helps control the circadian rhythm or the human body’s internal clock. Surprisingly, many of these neurotransmitters are also created by the cells and the trillions of microbes living in the gut. A large amount of serotonin is developed in the gut. Gut microbes also produce a neurotransmitter known as gamma-aminobutyric acid (GABA) which helps regulate feelings of fear and anxiety. Research studies in mice found that probiotics increase GABA and decrease anxiety and depression.
Is your memory noticeably declining? Are you having a hard time remembering names and phone numbers? Or is your ability to focus noticeably declining? If you’ve experienced any of these situations, you may ultimately be experiencing brain fog. What is Brain Fog? Brain fog is not a health issue but rather a symptom of other injuries or conditions. It is a cognitive dysfunction involving: - memory problems
- lack of mental clarity
- poor concentration
- inability to focus
Several people can also experience brain fog as mental fatigue. Based on the seriousness of brain fog, it may ultimately interfere with work, school, or any other regular tasks. However, it doesn’t have to be a permanent problem in your lifetime.
|



 Your new post is loading...
Your new post is loading...














Nerve irritation occurs when the nerves become irritated and sensitized. Chiropractic can diagnose and develop a personalized treatment plan. For answers to any questions you may have, please call Dr. Jimenez at 915-850-0900 or 915-412-6677